Understanding your FP34 Schedule of Payments
Published on: 5th May 2020 | Updated on: 6th May 2026
The Schedule of Payments is a document which provides contractors with a summary breakdown of reimbursement for drugs and appliances provided against NHS prescriptions including the fees payable for any additional NHS services provided for example, Advanced Services and any locally authorised payments from your NHS England Area team. Pharmacy contractors can expect to receive their Schedule of Payment (and eSchedules) from NHS Business Services Authority (NHSBSA) 5-working days before the payment date.
The look of the monthly Schedule of Payments (and eSchedules) has been updated recently. The new payment schedule has several improvements including:
- Inclusion of the advance service payment
- Breakdown of Pharmacy First payments, alongside activity data relating to this
- Total reimbursement and discount deduction split by generics/brands/appliances rates and between prescriptions and Pharmacy First Clinical Pathway items
- VAT information for products supplied under Pharmacy First Clinical Pathways
- The split of consumable and container allowances between prescriptions and Pharmacy First Clinical Pathway items
- The split of patient levies between prescriptions and Pharmacy First Clinical Pathway items
There are two different types of payment options for pharmacy contractors:
Early advance payment (FP34c submitted by 5th of the following month)
From November 2021, all contractors can access advance payments around 20 days earlier by submitting your FP34Cs using the Manage Your Service (MYS) portal no later than 5th of the month following that in which supply was made.
The 100% advance payments (for early and current timetables) will continue to be based on the items declared on the FP34C and the latest available Average Item Value (AIV) for that pharmacy, less the value of prescription charges declared on the submission document. Contractors must include their paper Account Identifier Document and dispatch it alongside their bundle of paper prescriptions. No advance payment will be received for very late submissions. The final reconciliation payment date remains unchanged i.e. this will be paid on the 1st working day of the month approximately two months after contractors have submitted the appropriate FP34C form and prescriptions for pricing.
The table below shows the earlier advance payment timetable dates for prescriptions dispensed over the next 12 months. For example, if submission is secured by the 5th of the month following that in which supply was made contractors will receive an earlier advance payment from November 2023 (starting for October’s prescriptions). For the dispensing month of October 2023, a contractor will be required to submit their FP34C declaration during the first 5 days of November 2023 to receive an early advance payment on 11 November.
The table also shows final deadline submission to qualify for normal advance:
| Dispensing Month | Jan | Feb | Mar | Apr | May | Jun | Jul | Aug | Sep | Oct | Nov | Dec |
| Submission deadline via MYS to receive early advance payment | 5th Feb | 5th Mar | 5th Apr | 6th May* | 5th Jun | 5th Jul | 5th Aug | 5th Sept | 5th Oct | 5th Nov | 5th Dec | 6th Jan 2026* |
| Earlier advance payment date (4 working days after submission deadline) | 11th Feb | 11th Mar | 10th Apr | 12th May | 11th Jun | 10th Jul | 11th Aug | 11th Sep | 9th Oct | 11th Nov | 11th Dec | 12th Jan 2026 |
| Pay date for reconciled prescriptions | 1st Apr | 1st May | 30th May | 1st Jul | 1st Aug | 1st Sep | 1st Oct | 31st Oct | 1st Dec | 31st Dec | 31st Jan 2026 | 27th Feb 2026 |
*Note – In months where one or more bank holiday occurs during the first five days of the month, contractors will be given an extra day to submit their FP34C and dispatch their prescription bundle to the NHSBSA. For these months, the early advance payment date will remain as four working days from the extended FP34C submission deadline of the 6th.
Later payment (FP34c submitted after 5th of the following month)
An estimated 100% of the normal advance payment for prescriptions is made by the NHSBSA for prescriptions submitted one month earlier (dispensed two months earlier). Payments are made on the 1st of each month, where this falls on a weekend or bank holiday payment will be made on the working day prior. MYS is the only route for all monthly submissions. Contractors who submit their figures after the 5th of the following month, will NOT receive any earlier advance payments but instead will receive advance payments in accordance with the current payment timetable i.e on or around the 1st of the month following submission.
For example, June payment will comprise of the 100% estimated Advance payment for prescriptions submitted in May (dispensed in April) with the full value of the priced prescriptions less the recovery of the estimated 100% Advance payment for prescriptions submitted in April (dispensed in March). Normal payment option timeline:
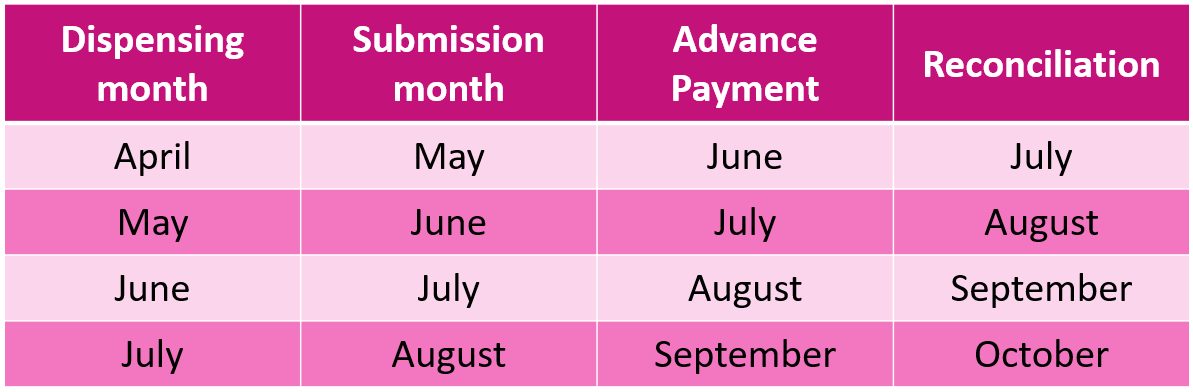
Pharmacy contractors can expect to receive their Schedule of Payment (and eSchedules) from NHSBSA 5-working days before the payment date. Contractors can view their monthly Schedule of Payments using the following options:
Paper
Schedule of Payment is sent by post to the pharmacy contractor’s specified address.
Electronic
eSchedule – NHSBSA produces electronic payment schedule data (called ‘eSchedule’) which pharmacy contractors can use instead of receiving a paper copy. The eSchedule is an electronic file that contains all of the data on the paper FP34 Schedule of Payments. Contractors will no longer receive a paper Schedule of Payments if they register for the eSchedule. For further information on eSchedules including how to register for the service, click here. eSchedules can be received alongside the paper FP34 and if you are satisfied with the data, at an agreed time, NHSBSA will stop sending paper FP34s.
Information Services Portal (ISP) – The Schedule of Payments can be viewed through the (ISP). You can still receive paper Schedule of Payments if you have registered for the ISP.
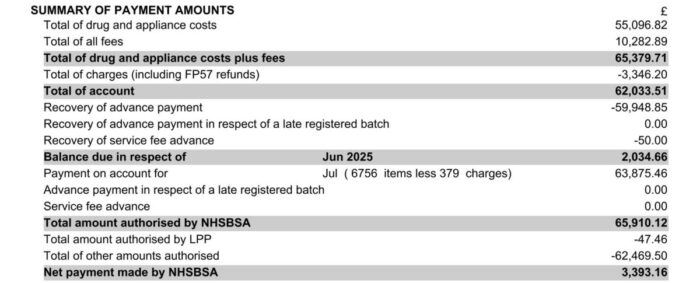

The ‘Summary of Payment Amounts’ shows how the ‘net payment’ is calculated by providing a breakdown of payments with the recovery of costs for that month.
The final Net Payment is calculated as:
Total of account minus ‘recovery of Advance payment’ (1) plus ‘payment on account for…’ plus ‘any other authorised amounts’ (3).
The ‘Summary of Payment Amounts’ includes the total value of drugs and appliances dispensed, fees and allowances received, and the value of the prescription charges retained by the contractor (i.e. prescription charges received minus refunds). This section also includes the following:
- The recovery of the Advance payment that was previously made in respect to this dispensing month. This is now being recovered as all items have been individually priced.
- Pharmacy owners receive service advance payment on the same day as the advance payment for dispensed prescriptions, provided they submit the claims on time. The following services are now included in the Advance payment calculation:
Service Included in Advance payment calculation from: Service fee advance Advance for product supplied Community Pharmacy Seasonal Influenza Vaccination Advanced Service (Adult Flu) September 2025 (Adult flu only)
(Childhood flu not yet included in the Advance payment)
Yes Yes COVID-19 vaccination service September 2025 Yes n/a Pharmacy First April 2025 n/a Yes Pharmacy Contraception Service (including Emergency Contraception) April 2025
(Emergency Contraception included from October 2025)Yes Yes Hypertension Case-Finding Service April 2025 Yes n/a Please note: Community Pharmacy England is working with DHSC and the NHS Business Services Authority (NHSBSA) to understand how the advance payments for specified services have been calculated. Advance payments for further services will be included in this ‘Service fee advance’ as NHSBSA’s pricing systems continue to be developed.
- The Advance payment for the next dispensing month (i.e. the payment on account for the following month, July in this case), which is the total number items declared on that month’s FP34C multiplied by the average item value (AIV). Your advance calculation will appear next to “Payment on account for” but if your batch is registered after advances have been calculated then your payment will appear next to ” Advance payment in respect of a late registered batch”. The calculation remains the same.
- The recovery of service fee advance that was previously made in respect to this dispensing month – similar to the recovery of advances paid for prescriptions.
- Any payments for local schemes such as locally commissioned Enhanced services.
If contractors have a positive payment under the Net Payment header, this means that payment is due unless a negative balance has been carried over from the previous month. If the payment has a negative value, the no payment is due and the negative balance will be carried forward and will be deducted from the next available payment.

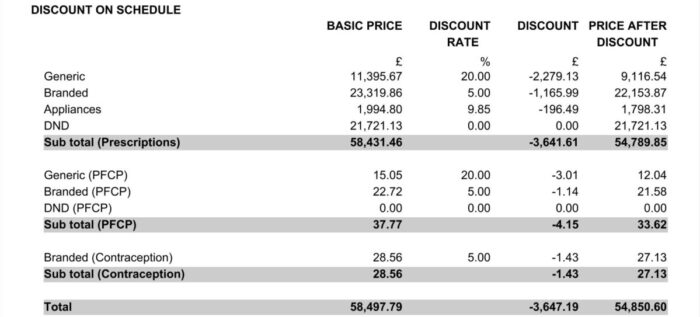
The ‘drug and appliance costs’ section lists the total value of drugs and appliances as priced by the NHSBSA. It states a sum for all products which attract discount deduction and also details the percentage discount that will be deducted from the total of basic prices at standard discount rate (further details on discount deduction can be found in Part V of the Drug Tariff). It provides a separate figure for zero discount items which have no discount deducted.
Other payments such as out of pocket expenses (OOP/XP), consumables and container fees are also listed.
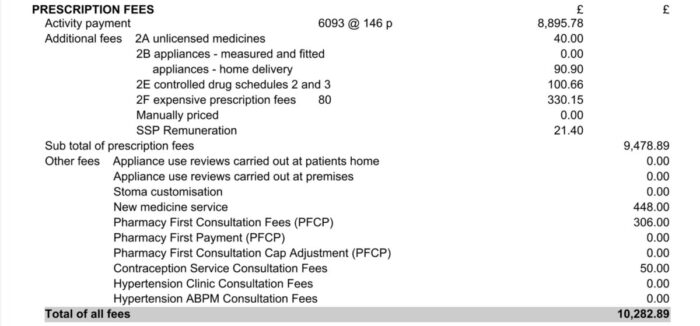

The ‘prescription fees’ section gives a breakdown of all the prescription related fees the contractor will be paid for the month. This includes the total value for the Single Activity Fee (displayed as activity payment) which is calculated by multiplying the SAF rate by the number of prescription items. Other fees outlined here include unlicensed medicines, appliances, Controlled drugs (Schedule 2 and 3) and expensive items. A breakdown of Flu Vaccination Service, Appliance Use Reviews (AURs), Stoma customisation, Pharmacy First (PCPF), Contraceptive Service Consultation, Hypertension Case-Finding Service, Lateral Flow Device (LFD) Service and New Medicines Service (NMS) is also included here.
Contractors can also find their Establishment payment in this section (for more details on Establishment payments, see Part VIA of the Drug Tariff).
For further information about the SAF see our Dispensing and Supply Factsheet: Understanding the Single Activity Fee
For more information on prescriptions requesting multiple flavours see our Multiple flavours factsheet

The charges section shows a more detailed breakdown of how many charges were deducted from the payment made to the contractor. It shows the number of charges and the rate of prescription charge, as well as the value of FP57 refunds, to provide the final amount to be deducted from payment by NHSBSA.
![]()
Here you will find a breakdown of payments authorised by your local NHS England Area team for providing local Enhanced services. Each local service will have their own scheme code. This section also details the pharmacy’s LPC levy.
For payments described on your Schedule of Payments as ‘Local Schemes’ you will have been notified separately by your NHS England local ICB which payment categories these relate to. NHS England have agreed a National Menu for Enhanced Services which can be found here.

The ‘details of other amounts authorised’ section includes various other payments a pharmacy contractor may be entitled to;
- Appliance Use Review (AUR)
- Covid-19 Vaccinations (please note, this is a locally commissioned service)
- Discharge Medicines Service
- Flu Vaccination Service
- Hypertension Case-Finding Service
- Lateral Flow Device (LFD) Service
- New Medicine Service (NMS)
- Pharmacy Contraception Service (PCS)
- Pharmacy First Service
- Smoking Cessation Service (SCS)
- Stoma Appliance Customisation
This section also details Pharmacy Access Scheme payments (if a pharmacy is eligible to receive this payment).
Recovery of Early Payment on Account – This relates to the early advance payment (value displayed on page 1 of the Schedule of Payments) that was paid earlier in the month, direct into pharmacy owner’s bank account, if the payment timetable was followed and the declarations were submitted via MYS by the 5th of the month. This payment is added to the schedule as a recovery to offset the positive entry on page 1, and therefore will stop the advance payment from being paid twice.
Foundation Trainee Pharmacist Training – a grant will be payable to pharmacy contractors who provide foundation trainee pharmacists (formerly known as pre-registration trainees) with the training experience needed by pharmacy graduates and certain undergraduates for admission to the General Pharmaceutical Council’s Register of Pharmacists. The grants are payable at annual rates in respect of each foundation training place filled by a pharmacy graduate or an undergraduate on a sandwich course recognised by the General Pharmaceutical Council as foundation training. Further information can be found in the Drug Tariff Part XIII.
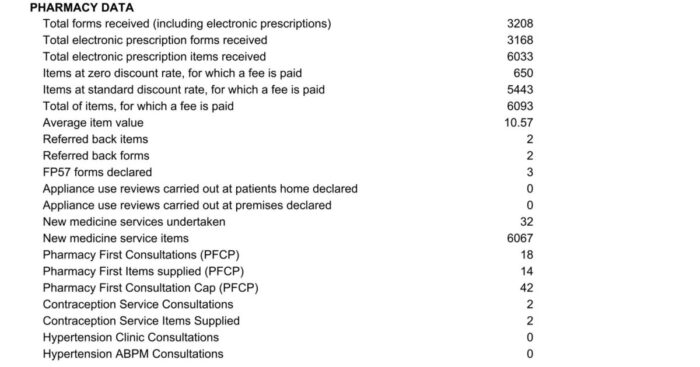
The ‘Pharmacy Data’ section details all prescription forms and items (both EPS and paper prescriptions) received by NHSBSA from the pharmacy. This is useful for pharmacy contractors to monitor and reconcile against their declaration/dispensing system totals. This section also details what the pharmacy’s average item value (AIV*) is. Any referred back forms and items are also displayed here.
*The AIV is calculated by taking the total cost of drugs and appliances, including all applicable fees, and subtracting the total value of other fees. This figure is then divided by the total number of relevant items supplied, comprising items for which a fee is paid, Pharmacy First items supplied, Contraception Service items supplied, and Influenza Vaccination consultation or vaccination items.
There are three product groups each with their own deduction rates which are applied to monthly reimbursement prices of the products in that group, as set out below:
| Group Name | Inclusion Criteria | Deduction Rate |
| Appliances | Part IX of the Drug Tariff | 9.85% |
| Generics | Category A of Part VIIIA of the Drug Tariff Category M of Part VIIIA of the Drug Tariff |
20% |
| Brands | Products not classified as an appliance or Products not classified as being listed in Categories A or M of Part VIIIA of the Drug Tariff |
5% |
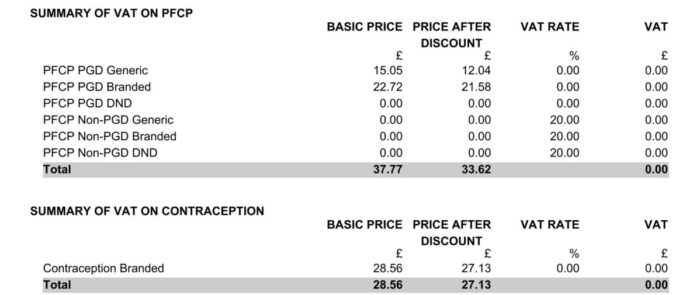
This section provides a breakdown of PFCP VAT payment that is displayed on page one.

This section shows a breakdown for Consumables and Containers for both regular prescriptions and PFCP. The total items and payment value should match the number of Consumables and Containers and payment for Consumables and Containers value on page one.

This section gives a breakdown of how many charges NHSBSA have deducted from your payment. The number of chargeable items shown should be similar to the number of chargeable items which you declared on your submission document (FP34C) for the dispensing month the Schedule of Payments relates to.
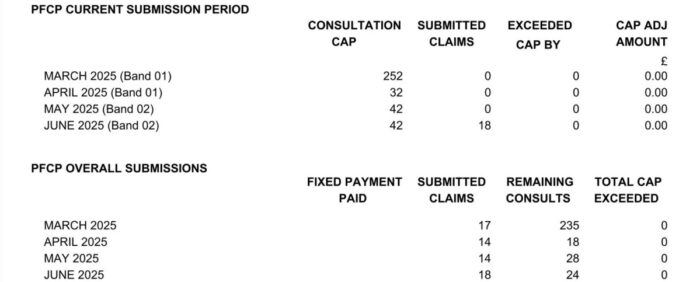
The ‘PFCP CURRENT SUBMISSION PERIOD’ table shows the breakdown of PFCP consultations claimed in the current submission period.
The ‘PFCP OVERALL SUBMISSIONS’ table shows the cumulative total of how many PFCP consultations were claimed, how many consultations remain before the cap has been reached and how many the cap has been exceeded by. If applicable, for the last four prescription months.

This section shows the number of items submitted to NHSBSA for pricing which have been switched between the exempt and chargeable groups.
NHSBSA transfer or ‘switch’ items between both exempt and chargeable groups when they identify items that are not in their correct group. The figure shown tells you how many items NHSBSA needed to transfer but does not always mean that NHSBSA have deducted a charge from your payment. You should always check the numbers and values in the ‘Charges’ section. Switched items will not include those which are EPS. EPS items are processed as declared.
To try and minimise loss from prescription switching, contractors are advised to monitor this closely, for example to ensure that staff are following standard operating procedures and ensuring that exemption declarations are completed as required.

This section shows the number and value of expensive items which were dispensed during the month, which have an item value of £100 or more. These values are important as fluctuations in the number or value of expensive items dispensed can have a significant impact on the average item value in a given month, and consequently the advance paid for the following month.
When checking the itemised list for expected payments the following aspects need to be considered:
- The itemised list is in value order with the largest value item at the top of the list;
- The prices quoted are the basic price of the quantity prescribed/dispensed and do not include any additional fees or adjustments due to broken bulk claims;
- If you have dispensed an item where the combined net ingredient cost of everything that made up that item is equal to or more than £100, that combined total will appear on the itemised list. e.g. if a Fluticasone item has a reimbursement value of £60 per pack, where one pack is prescribed, this would not appear in the expensive item section. If two packs were prescribed, the item total reimbursement value would be £120 and therefore this item would appear in the section;
- A product on the list may be described as an ‘exception Handler unspecified item’ or ‘exception handler discount not deducted Item’. These will include special order products not listed in dm+d;
- With products prescribed as ‘assorted flavours’ if the value of the quantity of an individual flavour dispensed does not exceed £100 then that flavour will not appear in the list.
If a product does not appear on the itemised list as expected, this does not necessarily mean that there has been incorrect payment. In these cases further enquiries can be made via the NHS Prescription Services Helpdesk on 0300 330 1349 or by email at nhsbsa.prescriptionservices@nhsbsa.nhs.uk
See our Dispensing Factsheet: Expensive items which defines what an expensive item is and provides guidance on the endorsement and submission of prescriptions for such items. It also explains how payments for expensive items are calculated by the NHSBSA and how contractors can reconcile these against their monthly Schedule of Payments (SoP) and/or Prescription Item Reports (Px reports).
This section contains guidance for pharmacy contractors in England.
Related resources
Prescription item report (PIR) and Information Services Portal (ISP)
How to access your Prescription Item Reports
Watch our webinar on-demand: Understanding your Schedule of Payments
Dispensing Factsheet: Expensive items
Temporary Safeguarding Payments
Dispensing and Supply Factsheet: Claiming for EPS prescriptions on time
Prescription payment and pricing accuracy – (this includes sections on Submission, Switching, Rechecks, Processing and Price accuracy)
NHSBSA Guidance on Pharmacy Payments
For more information on this topic please email comms.team@cpe.org.uk