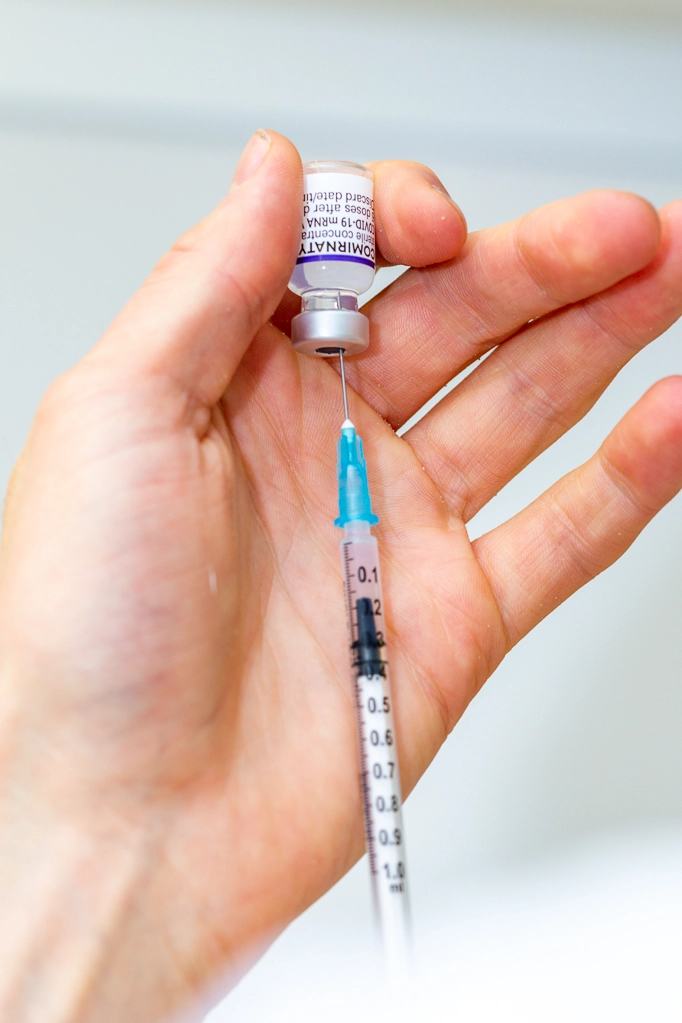
Smoking Cessation Service (SCS)
Published on: 23rd August 2021 | Updated on: 21st April 2026
This page contains information about the Smoking Cessation Service (SCS) which was commissioned as an Advanced service from 10th March 2022.
Latest updates
Updated SCS service spec and PGDs published ahead of changes to the service (18th December 2025)
In the 2024/25 and 2025/26 CPCF funding settlement, it was agreed that changes would be made to the Smoking Cessation Service (SCS) to allow suitably trained and competent staff to provide the service, alongside pharmacists and pharmacy technicians, who are currently able to undertake consultations.
It was also agreed that Patient Group Directions (PGDs) would be introduced to enable provision of varenicline and cytisinicline (Cytisine) under the service by both suitably trained and competent pharmacists and pharmacy technicians.
These changes to the service necessitate updates to the service specification and new PGDs for varenicline and cytisinicline (Cytisine).
We have been working with NHS England and DHSC on these documents and draft versions have now been published on the NHSBSA website.
Download the DRAFT documents from the NHSBSA website
These draft documents have been published to provide advance notice of the changes to the service for pharmacy owners and their teams, and additionally to support IT system suppliers in developing the necessary changes to their systems.
The commencement date for the revised service will be announced by NHS England in due course; a provisional start date has not yet been agreed.
Prior to the commencement date for the revised service, the final versions of the service specification and PGDs will be published on the NHS England website. From the commencement date, the updated documentation on the NHS England website must be used by all pharmacy owners providing the service, not the draft documents which have now been published.
For now, the service has not changed, and pharmacy owners and their teams must continue to provide the service in line with the current documentation published on the NHS England website.
Click on a heading below for more information
In January 2019, the NHS Long Term Plan (LTP) was published which said that the NHS would make a significant new contribution to making England a smoke-free society, by supporting people in contact with NHS services to quit based on a proven model, the Ottawa Model for Smoking Cessation (OMSC). The OMSC establishes the smoking status of all patients admitted to hospital followed by brief advice, personalised bedside counselling, timely nicotine replacement therapy (NRT) or pharmacotherapy, and follow-up of the patient after discharge. The NHS LTP also said that all people admitted to hospital who smoke would be offered NHS-funded tobacco treatment services by 2023/24.
In July 2019, Community Pharmacy England, the Department of Health and Social Care (DHSC) and NHS England agreed a five-year deal for community pharmacies, which included piloting a service to take stop smoking referrals from secondary care and then if successful, in Year 3 (2021/22) to commission such a service nationally.
In 2020/21 a Pharmacy Integration Fund pilot on smoking cessation began to test a new model of working in which community pharmacies managed the continuing provision of smoking cessation support initiated in secondary care following patient discharge from hospital.
The early findings from the pilot indicated that a consistent, national offer could be achieved through community pharmacy, and that it could create the capacity needed to enable NHS trusts to transfer patients for smoking cessation support into the community. The SCS was therefore added to the NHS Community Pharmacy Contractual Framework (CPCF) as part of Year 3 (2021/22) of the five-year CPCF deal.
Smoking rates have fallen significantly in the last 10 years, but smoking still accounts for more years of life lost than any other modifiable risk factor.
Around 5.7 million people or nearly 14% of the adult population in England were reported to smoke in 2019. Smokers see their GP over a third more often than non-smokers, and smoking is linked to nearly half a million hospital admissions each year.
The NHS Long Term Plan set a goal that by 2023/24, all people admitted to hospital who smoke will be offered NHS-funded tobacco treatment services. The plan committed to the adoption of the Ottawa Model for Smoking Cessation (OMSC), which has been evidenced across Canada to improve smoking quit rates by 11%.
As part of the OMSC, the smoking status of all admitted patients, is identified, followed by brief advice, personalised bedside counselling, timely nicotine replacement therapy and/or pharmacotherapy, and follow-up support for smoking cessation post-discharge.
To achieve successful smoking cessation, collaboration and an effective transfer of care are needed between secondary and primary care for all patients supported by the OMSC. Community pharmacy owners have the potential to deliver this primary care smoking cessation support, and to be part of this wider aim for the NHS which will significantly benefit the patients referred.
Aim and objective of the SCS
The aim of the SCS is to reduce morbidity and mortality from smoking, and to reduce health inequalities associated with higher rates of smoking with the objective of the service being to ensure that any patients referred by NHS trusts to community pharmacy for the SCS receive a consistent and effective offer, in line with NICE guidelines and the OMSC.
This service has been designed to enable NHS trusts to undertake a transfer of care on patient discharge, referring patients (where they consent) to a community pharmacy of their choice to continue their smoking cessation treatment, including providing medication and support as required. The ambition is for referral from NHS trusts to community pharmacy to create additional capacity in the smoking cessation pathway.
The service can only be provided by a pharmacist or pharmacy technician.
The service requirements are included in the service specification, which pharmacy owners must read before deciding whether to provide the service.
Download the patient flow diagram
Service Directions and Determination (March 2022)
The Pharmaceutical Services (Advanced and Enhanced Services) (Amendment) (England) Directions 2023 (published April 2023 – amended to allow pharmacy technicians to provide the SCS)
The Secretary of State Directions provide the legal basis for the provision of the service.
Community Pharmacy England Briefing 020/23: Updated guidance on the Smoking Cessation Service
Our Briefing provides additional guidance for pharmacy owners and their teams on the service.
The service officially commenced on 10th March 2022, however since this is an Advanced service, pharmacy owners are free to choose if they will provide the service and when they will start providing it.
Not all NHS trusts will immediately start to make referrals to the service; NHS England expect most to be making referrals within two years from the commencement date.
Before registering to provide the service, pharmacy owners need to consider the likelihood that they will receive sufficient referrals to make provision of the service practical and worthwhile. The starting point in making that assessment should be determining whether local NHS trusts are already making referrals to pharmacies by talking to your Local Pharmaceutical Committee (LPC). Where trusts have not yet started to make referrals, LPCs may have information available on the likely timing of them commencing over the next couple of years.
Pharmacies must have a consultation room in order to be able to offer this service, which meets the requirements in the Terms of Service. The consultation room must also have IT equipment accessible within the room to allow contemporaneous records of the consultations provided as part of this service.
If a pharmacy owner has had agreement from NHS England that their pharmacy is too small for a consultation room or a pharmacy (including distance selling pharmacies) does not have a consultation room, then they are not able to provide the service solely on a remote basis. The service is ordinarily intended to be provided face-to-face so this option must be available for patients.
If the pharmacist or pharmacy technician and patient agree that the service can be carried out remotely on an individual or ongoing basis, for example because the patient is housebound while recovering from surgery, this should be carried out via telephone or video call in circumstances where the conversation cannot be overheard, except by someone whom the patient wants to hear the conversation, for example, a carer. That may, for example, mean the pharmacist or pharmacy technician uses the consultation room to undertake the remote consultation. Further information on remote consultations can be found on our Virtual conferencing & remote consultations page.
To provide the service, pharmacy owners must have a carbon monoxide (CO) monitor (which is suitable for use with pregnant women) and sufficient disposable single patient use mouthpieces to meet the likely demand when providing the service via face-to-face consultations in the pharmacy. The minimum technical specification for a CO monitor that can be used for the service can be found in Appendix A of the service specification and details of monitors which meet this specification are available below. Monitors may also require parts of the monitor to be replaced regularly so pharmacy owners should ensure they are aware of these requirements and have sufficient replacement parts, as detailed in the CO monitor manual.
Pharmacy owners should ensure they are aware of the routine maintenance, specific cleaning and calibration requirements for the CO monitor as detailed in the CO manual that is provided with the CO monitor.
Currently available (in the UK) breath CO monitors for the SCS
The CO monitor must be appropriate for use on adult and/or pregnant patients. NHS England has provided the following information on devices currently available in the UK that meet the criteria for the service:
There are two choices of CO monitors for both pregnant and non-pregnant smokers. These are:
Bedfont: PiCObaby Smokerlyzer and Micro+ Smokerlyzer
MD Diagnostics: CO Check Baby + and CO Check (Pro) Baby
Equipment maintenance, calibration & cleaning
All CO monitoring equipment should be regularly checked and calibrated in accordance with the manufacturer’s instructions; these maintenance recommendations may vary between devices.
Infection prevention and control measures and cleaning must be carried out on all CO monitors as per the instructions of the manufacturer or supplier and in line with current infection prevention and control guidance. Detergent and disinfectant wipes can damage plastic surfaces of medical devices if they are not compatible with the surface material. In line with MHRA’s guidance, pharmacy owners are advised to only use cleaning products that are compatible with the device.
The SOP for the service must include the processes for cleaning, maintenance, validation and recalibration of the equipment used. Pharmacy owners can access additional guidance from the MHRA’s Managing Medical Devices guide.
To provide the service pharmacists and pharmacy technicians must have:
- Read and understood the operational processes to provide the SCS as described in the service specification;
- Successfully completed the following National Centre for Smoking Cessation and Training (NCSCT) courses and satisfactorily passed the assessments (where applicable):
-
- Stop Smoking Practitioner training and certification;
-
- Mental health and smoking cessation course;
-
- Pregnancy and smoking cessation course; and
-
- E-cigarettes: a guide for healthcare professionals course.
- Have read the NCSCT Standard Treatment Programme (STP), which will be used to support consultations.
Pharmacists and pharmacy technicians should also be aware of the availability of locally commissioned services and national support helplines/ groups; the Better Health quit smoking page includes information on getting daily email support, online communities and information on the National Smokefree Helpline.
Additional optional training
Pharmacists and pharmacy technicians wanting to undertake further training on smoking cessation can do so on an optional basis to support their own continuing professional development (CPD).
The Centre for Pharmacy Postgraduate Education has additional learning and links to further reading, which pharmacists, pharmacy technicians and other members of the team could consider accessing (please note, this is not a mandatory requirement for the service).
Pharmacy team training
Although the service must be provided by a pharmacist or pharmacy technician, it is important that the wider pharmacy team are aware of the SCS and how it will operate. You could consider:
- Holding a briefing session for your team;
- Providing them with the one-page overview (please see below) on how the service will work;
- Discussing as a team how you can work collectively to make the service a success; and
- Making sure team members are clear on the daily activity required, such as checking for referrals, diary management, etc.
Download our Briefing for pharmacy teams on the service
Standard operating procedure
Pharmacy owners must have a standard operating procedure (SOP) in place for this service covering provision of the service, which should include key contact details for the service; the process for maintenance and validation of the equipment used and infection prevention and control measures; and signposting to locally commissioned smoking cessation services. The SOP should be reviewed regularly and following any significant incident or change to the service. All pharmacy staff involved in the provision of the service must be familiar with and adhere to the SOP.
Various pharmacy support organisations provide template SOPs which their members can personalise for use in their pharmacy.
Signing up to provide the service
Pharmacy owners must notify NHS England that they intend to provide the service by completion of an electronic registration through the NHS Business Services Authority’s (NHSBSA) Manage Your Service (MYS) application.
Engagement with local GP practices and/or PCN colleagues
Prior to commencement of the service, it is advisable for pharmacy owners to engage with local GP practices and/or Primary Care Network (PCN) colleagues to make them aware the pharmacy will be participating in the service. Although GP practices cannot refer patients to this service, pharmacy owners will be sending them the outcome of the service provision for their patients who agree to participate in the SCS; therefore, it is important that they are aware of the reason for this.
A letter / email template to support pharmacy owners to notify GP practices that the pharmacy will be providing the service is available.
Download our GP letter/email service notification template (Microsoft Word)
Accessing referrals
Pharmacy owners should ensure that an appropriate number of staff are able to access the electronic referral system used by the trust to send referrals and/or the premises specific NHSmail account to ensure they are able to access referrals.
Promoting the service
NHS trusts are responsible for promoting this service to their eligible patients. The service should not be actively promoted to the public by pharmacy owners. The service is specifically for patients referred from NHS trusts who choose to continue their tobacco dependence treatment in community pharmacy following discharge from hospital, by committing to participate in the SCS. The service may not otherwise be used as an alternative to existing, locally commissioned specialist stop smoking support.
Patients presenting at the pharmacy without a referral having been received by the pharmacy are not eligible for the SCS and should be treated in the same way as other patients who present directly at the pharmacy for smoking cessation advice.
NHS website and DoS profile
The pharmacy’s NHS website profile and the Directory of Services (DoS) profile do not need to be updated to indicate that the service is provided as this is not a service that patients or NHS 111 can refer themselves/patients to.
Pharmacy owner checklist
Once a pharmacy owner has decided they wish to provide the service, our implementation checklist will guide you through the steps you need to take to prepare to provide the service.
Download our Smoking Cessation Service implementation checklist
Patients are only eligible to receive the service if the pharmacy has received a referral electronically from an NHS trust.
Inclusion criteria for the service
- People aged 18 years and older who have started treatment for tobacco dependence in hospital and have chosen to continue their treatment in community pharmacy after discharge; and
- This service does not exclude women who are pregnant or people who suffer from non-complex mental health problems although alternative local arrangements may already be in place for such people.
Exclusion criteria for the service
- Children and adolescents under the age of 18 years; and
- People who have completed a 12-week smoking cessation programme while in hospital as a result of an extended duration as an inpatient.
Clinically significant drug interactions
Although not considered an exclusion, the NHS Specialist Pharmacy Service (SPS) has compiled a list of drugs that have been identified as having a significant interaction with tobacco smoking:
Some of these may require dose adjustment or increased monitoring when patients change their smoking status.
Further advice includes:
- Certain drugs may require does adjustment.
- Close monitoring of plasma levels (where useful), clinical progress and adverse effect occurrence and severity is essential when patients change their smoking status.
- Patients taking narrow-therapeutic-index drugs should be monitored closely when any lifestyle modification is made.
- If the affected drug is prescribed under the supervision of a specialist, their input should be sought if the patient changes their smoking status.
Referrals
NHS trusts will identify patients who are smokers, provide a pre‑quit assessment, and start treatment. With consent, patients will be offered a referral to a pharmacy which is participating in the SCS (the patient will choose which pharmacy they wish to be referred to). The referral will be made using a secure electronic system or NHSmail following discharge from hospital.
The information which should be included in the referral is listed in Appendix C of the service specification.
All pharmacy staff involved in providing the service will need to understand how referrals are made and what IT systems to check for referrals. The IT systems will need to be checked regularly to see if the pharmacy has received any referrals.
If a patient presents at the pharmacy requesting smoking cessation advice, the pharmacy team may want to ask if they have been referred from an NHS trust for the service (in case the patient presents before the pharmacy has contacted the patient about their referral). If the patient confirms this to be the case, the pharmacy team should then check to see if a referral has been received.
If a referral has not been received
If a patient phones or presents in the pharmacy to arrange an appointment for the service, but a referral has not been received by the pharmacy, the following actions should be taken:
- Double check that they have recently been discharged from an NHS trust;
- Check with the patient the name of the pharmacy that they chose to be referred to;
- If the patient has presented at the correct pharmacy and confirms recent discharge from an NHS trust, re-check the electronic referral system and the pharmacy premises shared NHSmail account to ensure a referral has not been received;
- If no referral is found, contact the referring NHS trust and ask for the referral to be re-sent; and
- If the NHS trust advises that there is no referral for the patient, the pharmacist or pharmacy technician should ensure appropriate advice and/or signposting is provided to the patient to ensure they can access appropriate smoking cessation support, e.g. from the local commissioned stop smoking service.
Receiving referrals
When a referral is received, a member of the pharmacy team should contact the patient within five working days to confirm they want to access the service and arrange their first appointment (alternatively, the patient may contact the pharmacy as they should also have been advised by the NHS trust to contact the pharmacy within five working days). The pharmacy team should try to contact the patient on at least three occasions (the last of which must be on the fifth working day following receipt of referral). If the patient is not contactable or advises that they no longer wish to access the service, the NHS trust tobacco dependency team should be notified, and the referral should be closed.
If the patient advises that at this time, they do not wish to access stop smoking support, they should be offered details of alternative stop smoking support services that they could consider accessing in the future.
No payment can be claimed where there is no consultation with the patient.
If a patient advises that they do want to access the SCS, the patient should be offered a date for their initial consultation (ensuring that the consultation is soon enough to ensure the patient does not run out of their NRT before the appointment).
The SCS is intended to be provided as a face-to-face service. On occasion there may be a requirement to provide behavioural support, monitoring, or follow up remotely, for example, telephone or video consultations. Remote consultations may only be considered if they will meet the requirements of the service specification and the patient agrees to this approach.
If the patient is unable to travel to the pharmacy, they should ask a representative to collect the NRT on their behalf. Pharmacy owners are not expected to deliver NRT to patients as part of the SCS but should follow their usual practice to support patients in gaining access to medicines.
Consent
The service should be explained to the patient and verbal consent must be sought and recorded in the pharmacy’s clinical record for the service. This consent should cover the full provision of the service and patients should also be advised of the following information sharing that will take place:
- The sharing of information between the pharmacy and the patient’s general practice to allow appropriate recording of the details of the service in their general practice record (see appendix D of the service specification for the information that should be shared with the patient’s GP);
- The sharing of information about the service with NHS England as part of the service monitoring and evaluation;
- The sharing of information about the service with the NHSBSA and NHS England for the purpose of contract management and as part of post-payment verification; and
- The sharing of information with the NHS trust tobacco dependency team for the purpose of the NHS Digital smoking return (see appendix E of the service specification).
Pharmacists and pharmacy technicians should follow the consultation structure within the NCSCT Standard Treatment Programme (STP) as applicable to patients, which should include:
- Undertaking a CO test;
- Provision of behavioural support; and
- Supply of NRT – this will be initially determined by the details of NRT supplied at discharge from hospital. The pharmacy will supply a maximum of two weeks NRT at a time. As part of the consultation the suitability of the NRT should be reviewed and any changes agreed with the patient. The course length should not exceed 12 weeks treatment from the defined quit date. This includes any treatment supplied to the patient while in hospital and at the point of discharge.
Pharmacy teams should also consider other services that they offer, for example, the Hypertension case-finding service, that they could advise the patient about to see if they would be interested in also accessing other services.
Future appointment dates should be agreed at the initial consultation that overlap with the length of treatment supplied so the patient is not due to run out on the day of their appointment. Formal reviews must be held at four and twelve weeks post-quit; the agreed interim appointment cycle should coincide with these formal review dates.
CO readings
If the patients says that they have stopped smoking, but the CO test reading is higher than 10 parts per million (ppm) it may be that the patient is still smoking, and any further questions must be phrased sensitively to encourage an open discussion. However, patients should also be advised about possible CO poisoning and should be asked to call the free Health and Safety Executive gas safety advice line on 0800 300 363 if this is a possibility.
Supplying NRT
Patients will be discharged from the NHS trust with up to two-weeks supply of NRT. Following a remote or face-to-face consultation, the pharmacist or pharmacy technician should use their professional judgement to determine whether they may supply NRT in accordance with the requirements of the Human Medicines Regulations and the service specification.
A quantity sufficient for a maximum of two week’s treatment should be supplied to coincide with the next appointment. The supply of NRT should be entered onto the Patient Medication Record (PMR) and the NRT supplied should be labelled. The supply should be made free of charge to the patient; NHS prescription charges do
Further information on the NRT products which can be supplied as part of the service is available on the NHSBSA website under the ‘Nicotine Replacement Therapy list’ section.
Not supplying NRT
The pharmacist or pharmacy technician may decide it is not appropriate to make a supply of NRT. In deciding whether or not to make a supply, the pharmacist or pharmacy technician must consider the impact on the patient. If the pharmacist or pharmacy technician decides not to make a supply, it must be clearly explained, and the patient should ideally agree with this decision. If the patient requires support from another healthcare professional, the pharmacist or pharmacy technician must organise this for the patient.
Where no items are supplied to the patient, it is important that the reasons are captured within the clinical record for the service.
Onward referral when an item is out of stock
If the required NRT product cannot be supplied in time to maintain continuous treatment, the pharmacist or pharmacy technician should discuss alternative formulations with the patient that they could try, which would mean the patient could continue with the SCS from the same pharmacy. If the option of an alternative formulation is not acceptable to the patient, then agreement should be made with them for referral to another pharmacy providing the SCS. The pharmacist or pharmacy technician should contact the pharmacy and check that the product is in stock and that they are willing to accept the referral.
If the pharmacy does not have the items in stock, then the pharmacist or pharmacy technician should use their professional judgement as to the number of alternative pharmacies who are providing the SCS that should be contacted.
Once a pharmacy with the required product that can take the referral is found, the patient’s details should be transferred by forwarding the referral details to the new pharmacy via the electronic referral system (where this functionality exists) or via NHSmail. The patient should be provided with the details of the pharmacy to which they have been referred.
What to do if a patient does not attend for an SCS consultation
If a patient does not attend an agreed face-to-face or remote appointment, a member of the pharmacy team should attempt to contact the patient to rearrange the appointment. If the patient is not contactable, the NHS trust tobacco dependency team should be notified, and the referral should be closed.
The pharmacist or pharmacy technician should use their professional judgement to decide if it is appropriate to notify the patient’s GP; particular consideration should be given to people in vulnerable groups.
Information for patients
Pharmacists and pharmacy technicians should follow the consultation structure within the NCSCT STP and at the end of the consultation ensure they summarise the patient’s plan (by following the list in the NCSCT STP) and give them the opportunity to ask any questions.
Communicating with GP practices
The patient’s GP must be informed of the outcome of the service provision; appendix D of the service specification outlines the data that must be sent to the patient’s GP when the patient is discharged from the service.
Record keeping and provision of data to NHS England
Pharmacy owners will need to select and contract for an IT system that they can use to make their clinical records for the service. Information on IT systems that can support the service will be available soon.
NHS England and the NHSBSA are working with IT system suppliers to develop functionality that allows data from the clinical record of each service provision to be extracted and submitted to the NHSBSA’s MYS system via an application programming interface (API).
The information to be submitted via the API is specified in Appendix F of the service specification. This data will form the payment claim for the pharmacy owner and it will be used for post-payment verification (PPV) and evaluation of the service.
Clinical records of service provisions should be retained for an appropriate period of time, but for the purposes of PPV, they should be kept for a minimum of three years after the service takes place. As pharmacy owners are the data controller, it is for each pharmacy owner to determine what the appropriate length of time is, beyond two years that the clinical records are kept for. Decisions on this matter should be documented in the SOP and should be in line with Records Management Code of Practice for Health and Social Care.
NHS approved IT systems for recording SCS consultations and sharing data with the NHSBSA are due to be ready in the first quarter of 2024.
This development follows negotiations with NHS England and the Department of Health and Social Care where it has previously been agreed that IT support for CPCF clinical services will be updated to allow information on services provided and payment claims to automatically flow from pharmacy IT system to the NHSBSA.
This work has already been completed for several of the CPCS clinical services, with the development of application programming interfaces (API) between pharmacy IT systems and the NHSBSA’s Manage Your Service (MYS) portal.
NHS England have advised that the go-live date for the SCS API is Quarter 4 of 2023/24 (though one IT system supplier already has a live API).
Once the work at the NHSBSA and IT system suppliers is completed, pharmacy owners providing the services will need to use an approved pharmacy clinical IT system to keep their clinical records for the services and to submit data on the provision of the service and payment claims to MYS. At that time, the current manual claim processes for the services will be retired.
Find out more about IT support for all CPCF clinical services
If an API has been put in place by a pharmacy owner’s IT supplier, claims for payment for this service should be made monthly via the MYS portal.
The status of CPCF IT suppliers with alignment to the APIs is set out at our webpage about Pharmacy services IT requirements.
Where your IT system supplier does not currently have an API in place, an interim process will be used; further information on this process is available on the NHSBSA website.
Pharmacy owners providing this service will be eligible for the following payments:
- A set-up fee of £1,000 (which will be paid following registration on MYS to provide the service, having declared the pharmacy is ready to provide the service and relevant staff have undertaken the essential training specified in section 3 of the service specification and passed the e-assessments, where applicable).
- For each patient, a fee for:
-
- the first consultation of £30;
-
- each interim consultation of £10; and
-
- the last consultation of £40 (the last consultation may be at any point from and including the 4-week review up until the 12-week review).
- The products that may be supplied as part of this service are listed in the Drug Tariff Determination and only those products listed will be eligible for payment. The indicative reimbursement price will be the NHS list price of the reference product on the 8th of the month before. An allowance at the applicable VAT rate will be paid to cover the VAT incurred when purchasing the product supplied. The indicative price for reimbursement for each product that can be supplied as part of this service is based on a reference product as set out in the list available on the NHSBSA website.
Once your IT system supplier has an API in place for your IT system, the dataset to be reported to NHSBSA’s MYS portal is listed in Appendix F of the service specification. This will be collected automatically via the API for this service.
If a pharmacy owner wishes to stop providing the SCS, they must notify NHS England that they are no longer going to provide the service via the MYS platform, giving at least one months’ notice prior to the cessation of the SCS. Pharmacy owners will be asked for a reason as to why they wish to stop providing the service.
If a pharmacy owner de-registers from the service or ceases trading within 30 days of registration, they will not qualify for the £1,000 set up fee. In this event, if the £1,000 has already been paid back to the contractor, this money will be claimed back.
After de-registering from the service on the MYS portal, pharmacy owners will not be able to re-register for a period of four months from the final day of their 30 day’s notice.
Visit the Smoking Cessation Service Frequently Asked Questions page for FAQs on the service requirements.
Community Pharmacy England Briefing 020/23: Updated guidance on the Smoking Cessation Service
Template GP letter/email service notification template
Midlands and Lancashire Commissioning Support Unit
SCS Implementation resource pack
This resource pack provides guidance and suggestions on implementing the SCS for Trust Tobacco Dependence Teams, Local Pharmaceutical Committees (LPCs), community pharmacies, Integrated Care System (ICS) pharmacists, and Locality Tobacco Leads.
NCSCT resources
Standard Treatment Protocol
The National Centre for Smoking Cessation and Training (NCSCT) has published a bespoke Standard Treatment Programme (STP), which has been commissioned by NHS England for the SCS.
The original NCSCT STP provides guidance on delivering multi-session smoking cessation support. However, the new STP has been tailored for community pharmacists and pharmacy technicians offering the SCS; providing guidance on delivering tobacco dependence treatment to patients following discharge from hospital.
Pharmacists and pharmacy technicians offering the service will need to read the STP in full, as this is one of the training requirements specified in the service specification. However, the document is intended to be used as a reference during the different stages of consultations. It should be followed closely to guide pharmacists and pharmacy technicians to provide effective and evidence-based behaviour change techniques to give patients the best chance of quitting.
It is acknowledged that the document is a ‘long-read’, however it is intentionally designed to serve as a comprehensive guide that includes different scenarios and offers suggested ways to talk to patients and respond to common situations.
In addition to the STP, NCSCT has published the clinical checklists included in the STP as a separate document. This should allow pharmacists and pharmacy technicians to use them as an aide memoir to ensure they cover everything required in each consultation.
NCSCT would welcome feedback on the STP to allow them to make improvements to the STP. A feedback form is available via the link below for submitting comments.
View the NCSCT STP documents and feedback form
NCSCT also has a number of other useful resources including:
Stop smoking aids quick reference sheet
Pharmacists and pharmacy technicians may also be interested in the Secondary care factsheets, which summarise the relationship between cigarette smoking and specific diseases or conditions and the clinical benefits of quitting. They also cover what is known about intervening with these patient groups in the hospital setting, including the use of stop smoking medicines and referral to specialist stop smoking support.
At Community Pharmacy England, we are always keen to hear from pharmacy owners and their teams about how the provision of national pharmacy services is going, be that niggles with the way services are commissioned, a success story you want to share or something else.
Please click on the link below to share a success story where you have helped achieve a good outcome for a patient following a consultation for a national pharmacy service or to provide feedback on one of the services.
For more information on this topic please email services.team@cpe.org.uk