Pharmacy First: new FAQs and resource
As pharmacy owners and their teams continue to implement the Pharmacy First service, we have been responding to lots of your questions relating to the service at our recent online drop-in events, with the most frequently asked being added to our Pharmacy First FAQ webpage.
A selection of new questions added to the page can be found below and you can see the rest of our FAQs on the Pharmacy First FAQ page.
We have also published a new resource to assist you with providing online information sources to patients. When pharmacists are providing a consultation for one of the seven Pharmacy First clinical pathways, there are several leaflets/websites for patients to be pointed to which are listed in the PGDs and treatment protocol.
This new resource lists all the patient-facing leaflets/website links listed in the PGDs and treatment protocol, excluding the marketing authorisation holder’s patient information leaflets (hard copies will be available within the medicine’s packaging, with copies also being available from medicines.org.uk/emc). Hyperlinks to the leaflets/websites are listed, alongside QR codes for each leaflet/website so patients can scan this to access the leaflet/website link on their mobile phones.
Download Pharmacy First clinical pathways – online information sources for patients
Q. What should I do if the medicine specified in the clinical pathway is not available at the time of the patient consultation?
NHS England is currently considering the alternative options which could be offered to patients, where one of the medicines specified in the clinical pathway is not available. Those considerations will incorporate the need to avoid unnecessary use of antimicrobials in the circumstances where the treatment included in the pathway is not an antimicrobial (e.g. steroid nasal sprays).
Prior to NHS England providing further guidance on managing situations where a medicine is not available, the patient could be referred to another local pharmacy if it is likely that stock will be available elsewhere. If there is a general lack of availability of the product, the patient would need to be referred to their general practice, to be assessed and an alternative product prescribed, where clinically appropriate.
Q. Within the acute sore throat clinical pathway, do patients with a FeverPAIN score of 2 or 3 pass the Gateway point when they have a consultation with the pharmacist?
Yes. During the consultation, the pharmacist will be providing advice on self-care, including pain relief, and they will also be explaining to the patient that an antibiotic is not appropriate in their circumstance. They will also advise the patient to return if there is not improvement in 3-5 days. A clinical record for that consultation will be made to support any future consultations with the patient, and the consultation will pass the Gateway point, meaning a consultation fee will be paid.
Q. Where a clinical pathway advises that the patient should return for a further consultation in certain circumstances (e.g. Sore throat FeverPAIN score 2 or 3) will another consultation fee be paid for the second consultation?
Yes.
Q. Will the Pharmacy First consultation fee be paid for consultations with self-presenting (walk-in) patients who do not pass a Gateway point in the relevant clinical pathway?
No. For self-presenting patients, a fee will only be paid where the consultation is provided and the patient’s condition/situation passes a Gateway point in the clinical pathway. The discussions with these patients will incur a cost for pharmacy owners, which is a concern for Community Pharmacy England and is one of the reasons we negotiated the £1000 monthly payment which will be paid to pharmacies providing the service, subject to them meeting the minimum clinical pathway consultation numbers set out in the Drug Tariff.
If a patient is referred to the service, e.g. by a general practice, if they do not pass a Gateway point in the clinical pathway, the patient can still have a consultation under the minor illness consultation part of the service and a consultation fee will be paid for that.
Q. Do NHS prescription charges apply where the patient receives a medicine as part of the service?
Yes. The normal prescription charge rules apply to medicines or appliances supplied under the service, whether via the urgent medicines supply part of the service or the seven clinical pathways. The Pharmacy First IT system will print off a prescription token and the patient should complete the relevant parts of the reverse of the form to claim exemption from the prescription charge or to indicate they have paid the NHS prescription charge.
Q. What do I do with the prescription tokens patients have completed when a medicine was supplied as part of the service?
Where urgent medicines or appliances are supplied as part of an Urgent Medicine Supply referral the completed dispensing tokens should be sent to the NHSBSA as part of the month-end submission, clearly separated within the batch and marked ‘PF UMS’.
Where medicines are supplied as part of a Clinical Pathway consultation, the completed dispensing tokens should be sent to the NHSBSA as part of the month-end submission, clearly separated within the batch and marked ‘PF CP’.
Q. The service specification references the need for pharmacies (apart from Distance Selling Pharmacies) to have an otoscope. Do pharmacies need any other equipment?
The otoscope is the only equipment specified by the service specification, but pharmacy owners may want to consider having a thermometer which can be used to measure patients’ temperatures during consultation. Tongue depressors and a small torch may also help with examination of the throat, within the sore throat pathway.
Q. How can general practices refer patients to a pharmacy for a minor illness or clinical pathways consultation?
Referrals need to be sent to the patient’s chosen pharmacy in a secure, electronic manner that complies with the standards laid out in the NHS CPCS Technical Toolkit. There are several compliant ways in which referrals can be sent from within general practice IT systems, ‘bolt-on’ systems or NHSmail can be used. NHS England is currently in the process of developing guidance on the Pharmacy First service for general practices, but in the meantime, practices may want to refer to NHS England’s NHS community pharmacist consultation service toolkit for GP PCN staff. General practice staff could also contact their ICB’s community pharmacy clinical lead for further assistance on how this topic and in many cases, the Local Pharmaceutical Committee may also be able to provide advice to the practice.
Q. How can healthcare professionals identify pharmacies providing the service, so they can refer patients to them?
More than 95% of pharmacies are signed up to provide the service and healthcare professionals can check pharmacy profiles in NHS Service Finder to identify which pharmacies are registered to provide the service. Additionally, if general practice teams use EMIS local or PharmRefer to make referrals to the service, participating pharmacies are shown in those systems.
Q. Can Pharmacy First consultations be provided remotely?
Where it is clinically appropriate to do so, minor illness consultations (referrals) and urgent medicines supply consultations (referrals) can be undertaken via telephone/audio or video consultation by a pharmacist who is on the pharmacy premises.
Similarly, where it is safe to do so, clinical pathways consultations can be conducted via good quality video consultation by a pharmacist who is on the pharmacy premises. Remote clinical pathways consultations can only be provided via a good quality video consultation – they cannot be provided by a telephone/audio consultation.
The various options for providing consultations are set out in the table below.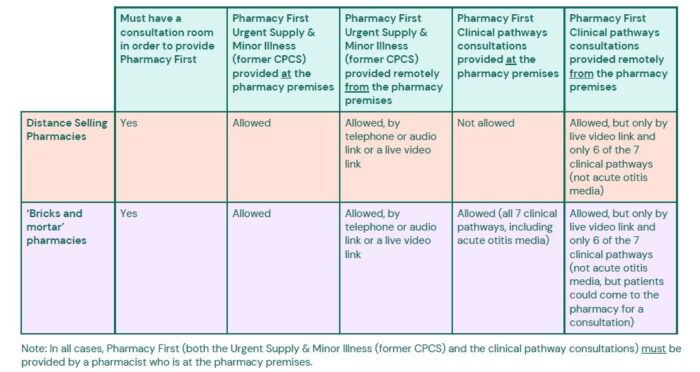
Q. Is there any advice available on which systems to use for video consultations with patients?
Our Virtual conferencing & remote consultations webpage provides advice and links to further information on this topic.
Q. When can I claim for service provisions made on the 31st January 2024 (the first day of the Pharmacy First service)?
Any service provisions on 31st January 2024 will be included in the February 2024 service claim.









