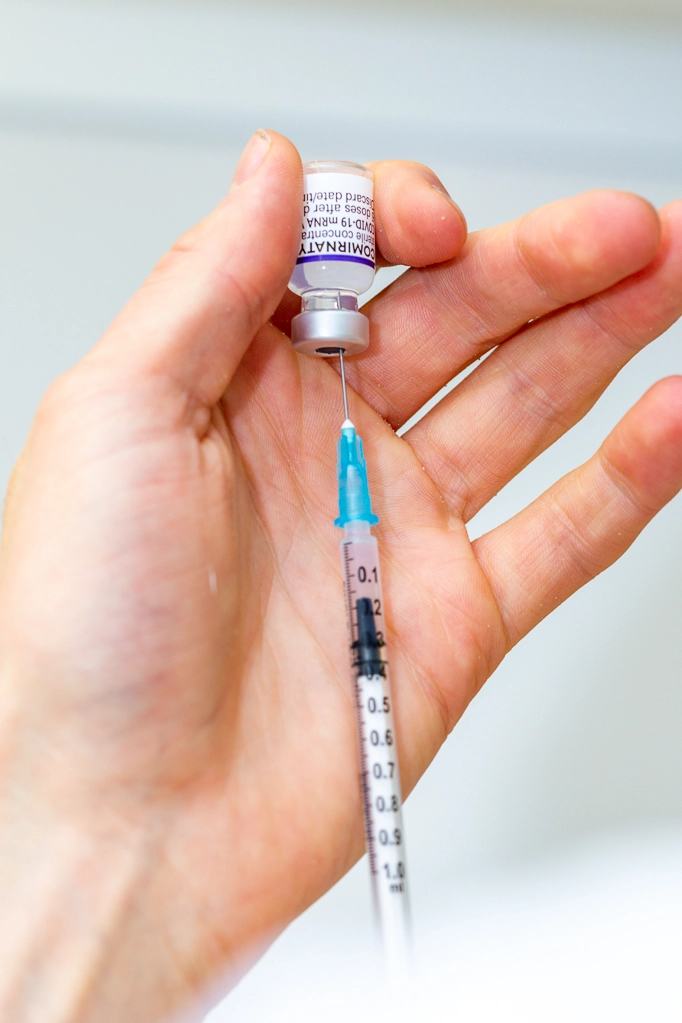
Seasonal Vaccination Services – COVID-19 and Adult Flu
Published on: 6th February 2026 | Updated on: 19th March 2026
This page contains information about the Seasonal Vaccination Services (COVID-19 and adult flu).
Via this new Advanced service, pharmacy owners can offer both COVID-19 and adult flu vaccinations, or just adult flu. From 1st April 2026, this new service replaces the previously commissioned COVID-19 vaccination Enhanced and Adult Flu vaccination Advanced services.
The service will initially support the administration of COVID-19 vaccinations to eligible cohorts as part of the Spring 2026 COVID-19 vaccination campaign.
COVID-19 vaccinations for the Spring 2026 campaign will commence on 13th April 2026 and will end on 30th June 2026.
Later in the year, pharmacy owners providing the service will be able to provide COVID-19 and adult flu vaccinations or solely adult flu vaccinations during the autumn/winter 2026/27 vaccination season.
Information about the previously commissioned COVID-19 Vaccination Enhanced service can be found in the archive section of the National Enhanced Services hub page.
Latest news
C-19 vac: Spring programme PGD published
NHS England has authorised and published the patient group direction (PGD) for use in the Spring 2026 COVID-19 vaccination campaign.
Read our news story highlighting its publication
Download the Spring 2026 COVID-19 vaccination PGD
Seasonal vaccination spring 2026 programme guide published
NHS England have published a guide to support vaccinations sites who intend to participate in the seasonal spring 2026 programme for COVID-19 vaccination.
The guide outlines how providers should deliver the Spring 2026 COVID‑19 vaccination programme, including operational processes, eligible groups, system usage, supply arrangements, and payment mechanisms.
Read our news story highlighting publication of the programme guide
Annual flu letter for 2026/27 published
- There are no changes to the eligible cohorts for the 2026/27 season compared to the last season.
- From 1st September 2026, pharmacies will be able to vaccinate pregnant women.
- Then, from 1st October 2026, vaccination of the other adult cohorts will commence.
- There are two changes to the recommended vaccines that pharmacy owners will need to consider when finalising their orders; and
- There is a reinforcement of the circumstances when the egg-based inactivated influenza vaccine (IIVe), can be used.
Read more in our news story on the publication of the annual flu letter
Click on a heading below for more information
The aims of the Seasonal Vaccinations Service are to:
- Protect those who are most at risk of serious illness or death should they develop COVID-19 and/or flu;
- Sustain and maximise the uptake and co-administration of COVID-19 and adult flu vaccinations to patients by continuing to build the capacity of community pharmacies as an alternative to general practice attendance; and
- Provide more opportunities and improve convenience for eligible patients to access COVID-19 vaccinations and adult flu vaccinations.
Immunisation is one of the most successful and cost-effective health protection interventions and it is a cornerstone of public health. High immunisation rates are key to preventing the spread of infectious disease, complications and possible early death among individuals and protecting the population’s health through both individual and herd immunity.
The impact of COVID-19 and flu on the NHS and social care continues to be significant. Those most at risk from flu are also most vulnerable to COVID-19, so, vaccination continues to be one of the most effective interventions the NHS has to reduce pressure on the health and social care system particularly during the winter months.
Background information on COVID-19 vaccinations in community pharmacies
During the COVID-19 pandemic, over 1,500 community pharmaces were involved in vaccinating patients and health and care workers under a Local Enhanced Service against coronavirus alongside vaccination centres, hospitals and Primary Care Network (PCN) sites.
In December 2020, the NHS commenced its COVID-19 vaccination programme. There were three types of vaccination site:
- Vaccination centres, using large-scale venues;
- Hospital hubs, using NHS Trusts across the country; and
- Local vaccination services, made up of sites led by general practice teams working together in primary care networks (PCN) and community pharmacy sites.
Through each of the previous phases of the vaccination programme, each NHS region, working with their integrated care systems (ICS), had defined the mix and number of sites required based on local demographics.
Pharmacies were central to the Government’s COVID-19 response, and figures from NHS England, in January 2022, showed just how significant a contribution they made to vaccination efforts: in the previous 12 month to January 2022, which marked the one-year anniversary of the sector providing COVID-19 vaccinations, more than 22 million vaccinations were administered by community pharmacy-led COVID vaccination sites. NHS England also highlighted a 50% increase in the number of pharmacies delivering COVID-19 boosters since October 2021.
The vaccination service was first commissioned as a Local Enhanced Service by NHS England regional teams in consultation with Local Pharmaceutical Committees. It was commissioned where there was a local need, for example where there was a gap in service provision or a need for additional capacity, and where pharmacy owners were able to meet the key designation requirements.
Those pharmacy owners selected as designated sites played a critical role in the success of Phase 1 (the vaccination of patient JCVI cohorts 1-9) and Phase 2 (the vaccination of patient JCVI cohorts 10-12) of the COVID-19 vaccination programme. Through their strong local relationships, community pharmacies helped to tackle vaccine inequalities and improve vaccination take-up.
The Phase 3 programme in 2021, was provided alongside the seasonal influenza vaccination programme, which runs each autumn.
In December 2021, provisions were made within the NHS (Pharmaceutical and Local Pharmaceutical Services) Regulations 2013 for a new type of Enhanced service, the National Enhanced Service (NES). Under this type of service, NHS England commissions an Enhanced service that is nationally specified. This requires NHS England to consult with Community Pharmacy England on matters relating to the service specification and remuneration for the service.
This differs from a LES that is locally developed and designed to meet local health needs and for which NHS England would consult with Local Pharmaceutical Committees. A NES allows the agreement of standard conditions nationally, while still allowing the flexibility for local decisions to commission the service to meet local population needs, as part of a nationally coordinated programme.
Phase 5 of the vaccination service, the Autumn 2022, Spring 2023, Autumn/Winter 2023/24 and Spring 2024 booster programmes, as well as the September 2024 to March 2026 campaigns were all commissioned as a NES.
On 30th May 2024, NHS England opened a new expression of interest (EOI) process for pharmacy owners that wished to take part in the COVID-19 vaccination service campaigns between September 2024 and March 2026.
The multi-campaign approach meant more pharmacies were able to participate. This removed the additional administrative burden of repeated EOIs before the start each campaign and unified the EOI process and requirements for all providers.
Background on adult flu vaccinations in community pharmacies
Community pharmacy owners has been providing flu vaccinations under a nationally commissioned Advanced service since September 2015.
During the 2024/25 season, for the first time adult groups (excluding pregnant women) were eligible for vaccination from 3rd October, rather than 1st September as in previous seasons. Therefore, data from UKHSA for those aged 65 years and over, and those aged under 65 years in clinical risk groups, is not comparable with previous seasons. As in previous seasons, pregnant women were eligible from 1st September.
Data from 1st September 2024 to 28th February 2025 in England, indicates that the NHS vaccination service vaccinated:
- 74.9% of those aged 65 years and over, compared to 77.8% in 2023/24;
- 40% of those in the under 65 years in one or more clinical risk groups, compared to 41.4% in 2023/24; and
- 35% of pregnant women, compared to 32.1% in 2023/24.
The Government continues to want the influenza programme to demonstrate a 100% offer and aim to equal or improve on the previous years uptake for each eligible group.
The potential for co-circulation of influenza, COVID-19 and other respiratory viruses could add significant pressures in the NHS. This co-circulation could add to or prolong the overall period for which respiratory viruses circulate in sequence. Vaccination, therefore, helps the health and social care system manage winter pressures by helping to reduce demand for GP consultations and likelihood of hospitalisation.
Pharmacy owners do not have a fixed patient list from which to undertake call and recall activities, however, pharmacy owners are encouraged to proactively offer influenza vaccination to any patient they identify as being eligible to receive it should the patient present in the pharmacy for any reason.
Service specification
Service specification for the seasonal vaccination services – COVID-19 and Influenza Vaccination Advanced services 2026/27
The service specification describes the requirements for provision of the services and it is essential reading for all pharmacists, pharmacy technicians and other vaccinators providing the service.
NHS England Seasonal Vaccination Provider Programme Guide (Futures platform)
System letter confirming the publication of the Advanced service specification
This letter summarises the key changes to the COVID-19 and adult flu service specification for 2026/27.
It includes details of the item of service fees for COVID-19 and adult flu vaccinations, the service registration process and deadlines, and changes in service requirements pharmacy owners should be aware of.
National annual flu letter
This confirms the timings, eligible cohorts and reimbursable vaccines for the 2026/27 flu vaccination season.
Patient Group Directions and National protocols
UKHSA produces the Patient Group Directions (PGD) and the national protocols that provide the legal mechanism for administration of COVID-19 and adult flu vaccines under the service.
PGDs
Patient Group Directions for COVID-19 vaccines (updated 17th March 2026)
These PGDs provide one of the legal mechanisms for administration of COVID-19 vaccines under the service.
A national Flu TEMPLATE Patient Group Direction (PGD) has been used by NHS England regional teams to create the PGD authorised for use within their region.
Copies of the regional PGDs can be found via the links below. These regional PGDs provide one of the two legal mechanisms for administration of flu vaccine under the service; pharmacy owners need to use the locally authorised PGD for the region in which their pharmacy is located.
- East of England – NHS England — East of England » Patient group directions
- London – NHS England — London » Immunisations
- Midlands – NHS England — Midlands » Patient Group Directions
- North East and Yorkshire (including North Cumbria) – NHS England — North East and Yorkshire » Patient Group Directions Yorkshire and the Humber
- North West – Lancashire, South Cumbria, Cheshire and Merseyside– NHS England – North West Inactivated Influenza Vaccine v14.0 PGD_FINAL
- North West – Greater Manchester – Greater Manchester Integrated Care Board (ICB) has authorised a PGD for use in Greater Manchester and this has been emailed to pharmacies by the ICB.
- South East – NHS England — South East » South East Patient Group Direction
- South West – NHS England — South West » NHS England South West – Patient Group Direction
The practitioners who can legally administer under the PGDs will be listed in the Qualifications and professional registration section of the PGD and this will mirror the groups of practitioners authorised to supply or administer medication via a PGD under current legislation. Any listed practitioners must provide the service under the oversight of the Responsible Pharmacist at the pharmacy.
The PGDs cannot be used to authorise administration of vaccines under any other NHS or private services.
Appropriately trained practitioners, who will administer vaccines under the authority of the PGDs must:
- Download a copy of the latest version of the PGD from the NHS England website;
- Read the PGD and ensure they fully understand its content, including the eligible patient groups, the inclusion and exclusion criteria and the record keeping requirements; and
- Print off a copy of the PGD and complete the Practitioner declaration to confirm they have read and understood the content of the PGD and that they are willing and competent to work to it within their professional code of conduct – if there is more than one practitioner in the community pharmacy or working with the community pharmacy who will be providing the vaccination service, one copy of the PGD can be printed and all practitioners can complete the practitioner declaration on this one copy.
The Authorising Manager declaration must then be completed. The Authorising Manager’s role is to confirm the practitioner(s):
- Is/are aware of the service specification and requirements for provision of the service;
- Have demonstrated their competence to provide the service; and
- Has/have the organisation’s approval to provide the service.
In certain circumstances, for example, a community pharmacy where the pharmacist who will administer vaccines is also the superintendent pharmacist or pharmacy owner, it may be necessary for the authorising manager to be the same person as the practitioner, though this situation should be avoided wherever possible.
These steps must be completed before an individual practitioner is authorised to administer flu vaccines as part of the service.
National protocols
National Protocols for COVID-19 vaccines (updated 7th March 2025)
These protocols provide the legal mechanisms for the administration of COVID-19 vaccines by appropriately trained persons in accordance with regulation 247A of the Human Medicines Regulations 2012 (HMR 2012), inserted by The Human Medicines (Coronavirus and Influenza) (Amendment) Regulations 2020.
National protocol for inactivated influenza vaccine 2025/26 (published 28th July 2025)
This protocol provides another legal mechanism for administration of flu vaccine under the service by appropriately trained persons in accordance with regulation 247A of the Human Medicines Regulations 2012.
A national protocol is a legal mechanism for the supply or administration of POMs, which was put in place following amendment of the Human Medicines Regulations during the COVID-19 pandemic. They were originally only intended to be used during a pandemic, but that approach has now been amended, so they can continue to be used outside of pandemic periods.
The protocol allows those who are registered healthcare professionals who cannot operate under a PGD, and those who are not registered healthcare professionals, in the context of the vaccination service being provided, to safely administer a licensed vaccine. The protocols for vaccines are developed by UKHSA and are very similar to a PGD.
The protocol provides the flexibility to define the training and competence requirements of vaccinators. It also allows the process of administration to be split into its component parts, i.e. clinical assessment and consent, preparation of the vaccine (not required for flu vaccine) and administration of the vaccine. This allows wider use of workforce skill mix to support the provision of the vaccination service. All these stages can be done by one competent person (the registered healthcare professional), but these tasks can also be split with each person trained and authorised to complete their specific task as defined in the protocol. The clinical assessment and consent process must be undertaken by a registered healthcare professional.
The choice of whether to operate under a protocol is the decision of the pharmacy owner. Pharmacy owners using the national protocol are responsible for ensuring:
- Those persons involved in the service or elements of the service are trained and competent to safely provide the activity they are employed to provide under the protocol;
- As a minimum, competence requirements stipulated in the protocol under Characteristics of staff must be adhered to;
- They and registered healthcare professionals have adequate and appropriate indemnity cover;
- Persons must be authorised by name to work under the protocol;
- The staff characteristics for the activity being undertaken are met;
- Practitioners make a declaration of competence and are authorised in writing. This can be done by completing Section 4 of the protocol or maintaining an equivalent electronic record;
- A clinical supervisor, who must be a pharmacist, doctor or nurse, must be present and take overall responsibility for provision of vaccination under the protocol at all times and be identifiable to service users; and
- Any time the protocol is used, the name of the clinical supervisor taking responsibility and all the people working under different stages of the protocol must be recorded for the session.
The clinical supervisor has ultimate responsibility for safe care being provided under the terms of the protocol. Staff working under the protocol may be supported by additional registered healthcare professionals, but the clinical supervisor retains overall responsibility. Staff working to the protocol must know who the clinical supervisor is at any time and only proceed with their
authority. The clinical supervisor may withdraw this authority for all members of staff or individual members of staff at any time and has authority to stop and start service provision under the protocol as necessary. Every member of staff has a responsibility to, and should, report immediately to the clinical supervisor any concerns they have about working under the protocol in general or about a specific individual, process, issue or event.
Appropriately trained practitioners or staff, who will be authorised to work under the authority of the national protocol must:
- Download a copy of the latest version of the national protocol from the GOV.uk website;
- Read the protocol and ensure they fully understand its content and the appropriate stages that they are expected to be able to provide; and
- Print off a copy of the protocol and complete the Practitioner/staff declaration to confirm they have read and understood the content of the protocol and that they are willing and competent to work to it under the supervision of the clinical supervisor. If there is more than one practitioner/staff member in the community pharmacy or working with the community pharmacy who will be providing the Flu Vaccination Service using the protocol, one copy of the protocol can be printed and all practitioners/staff can complete the practitioner/staff declaration on this one copy.
The Authorising registered healthcare professional declaration must then be completed. The individual taking on this role must be familiar with the competence required by all aspects of the protocol. The role is to confirm the practitioner(s) and staff:
- Is/are aware of the service specification and requirements for provision of the service;
- Has demonstrated their competence for the role and completed the necessary documentation; and
- Has/have the organisation’s approval to provide the service.
In certain circumstances, for example, a community pharmacy where the pharmacist who will administer vaccines is also the clinical supervisor and the authorising registered healthcare professional, it may be necessary for them to make a self-declaration of competency.
These steps must be completed before an individual practitioner or staff member is authorised to administer flu vaccines as part of the service. Pharmacy owners using this protocol should retain copies, along with the details of those authorised to work under it, for 10 years after the protocol expires.
Vaccine Group Directions
The legislation which enabled the development of National Protocols for the administration of COVID-19 vaccine lapses on 31st March 2026, but the Government has consulted on the introduction of a new, similar legal mechanism for the administration of vaccines – the Vaccine Group Direction – which will continue to enable suitably trained and competent registered and non-registered staff to participate in the programme.
Subject to the passage of legislation through Parliament, the COVID-19 Vaccine Group Direction for the spring programme is expected to be published on 1st April 2026.
Service start dates and duration
As the service combines the COVID-19 and adult flu service, details of the individual campaign timings for each aspect of the service will be confirmed via system letters.
COVID-19 spring 2026 programme
Vaccination should begin from 13th April 2026 and end on 30th June 2026. Priority should be given to care homes for older adults and eligible housebound patients.
Autumn/winter 2026/27 programme
The timings for the service are set out in the Annual flu letter:
- From 1st September 2026, pharmacies will be able to vaccinate pregnant women; and
- From 1st October 2026, vaccination of the other adult cohorts can commence.
Payment to all providers, will only be made for flu vaccinations administered from the service commencement date onwards. NHS England asks that following the service commencement date, pharmacy owners should maximise administration of flu vaccines by 30th November 2026.
The service will close on 31st March 2027.
Eligible patients
Pharmacy owners must ensure there are appropriate mechanisms in place to confirm each patient’s eligibility prior to the administration of a vaccine regardless of the route through which the patient has presented for their vaccination.
COVID-19 spring 2026 programme
Following the government’s acceptance of the Joint Committee on Vaccination and Immunisation advice on eligibility for the spring 2026 COVID-19 vaccination programme, the announced and authorised eligible cohorts for the COVID-19 spring 2026 programme are:
- adults aged 75 years and over
- residents in a care home for older adults
- individuals aged 6 months and over who are immunosuppressed, as defined in COVID-19: the green book, chapter 14a.
Autumn/winter 2026/27 programme
The eligible patient cohorts will be confirmed in the annual flu letter when this is published.
Pharmacy owners are not authorised to administer vaccines to other patient groups outside the defined eligibility cohorts for each vaccination.
If a vaccine is administered to patients in other groups, the pharmacy owner will not be paid for that vaccination and the administration will have been undertaken outside the legal authority of the legal framework being used
Pharmacy owners who wish to provide the service, should first read the service specification to ensure they are able to meet NHS England’s minimum requirements as specified in the service specification.
Pharmacy owners who feel they can meet the requirements set out in the service specification and who are confident they can support access to the eligible patients will need to register to notify the commissioner that they intend to provide either:
- COVID-19 and adult flu vaccinations to patients; or
- Adult flu vaccinations to patients.
COVID-19 and adult flu vaccination service registration
Pharmacy owners who wish to provide COVID-19 vaccinations as well as adult flu vaccinations, must register by 11.59pm on 2nd February 2026 to receive supplies of COVID-19 vaccine ahead of the spring 2026 COVID-19 service commencement date.
Pharmacy owners must register by completing an electronic registration form:
Access the COVID-19 Vaccination Service electronic registration declaration form
Pharmacy owners can continue to register after 2nd February 2026 to provide COVID-19 vaccinations during the spring 2026 campaign, but they are not guaranteed to receive supplies of the COVID-19 vaccine for the start of the campaign.
Registrations submitted after 2nd February 2026 will receive access to systems before the new contract starts on 1st April or, after that date, within 10 days of submission.
The electronic registration form will be in place until 31st March 2026.
From 1st April 2026 onwards, pharmacy owners must use the NHS Business Service Authority’s (NHSBSA) Manage Your Service (MYS) portal to register to provide the service.
Where a pharmacy owner has registered to provide COVID-19 vaccinations and adult flu vaccinations for the spring 2026 campaign and has not subsequently deregistered, their details will be automatically registered on MYS for the autumn/winter campaign.
If the pharmacy owner only wants to provide COVID-19 vaccinations and adult flu vaccinations from the autumn 2026 campaign, they must register via MYS by 11.59pm on 31st July 2026 to receive supplies of COVID-19 vaccines ahead of the anticipated autumn 2026 service commencement date.
Pharmacy owners can register after 31st July 2026; however, it is not guaranteed they will receive COVID-19 vaccine in time for the COVID-19 vaccination commencement date.
The final deadline to register to provide COVID-19 vaccinations in 2026/27 is 11.59pm on 30th November 2026.
Adult flu vaccination service registration
Where a pharmacy owner wishes to provide only adult flu vaccinations, they will be able to register from 1st April 2026 on MYS.
The deadline to register to provide adult flu vaccinations for the 2026/27 campaign on MYS is 11:59pm on 30th November 2026.
If pharmacy owners do not register by this date, they will not be able to provide the service in the 2026/27 season.
Pharmacy owners must not administer vaccines until they have registered to provide the service, as they will not be eligible for payment for vaccines administered prior to service registration.
There are several conditions that are specified in the service specification which pharmacy owners must comply with prior to provision of the service. These include:
- Pharmacy owners must be satisfactorily providing all Essential Services and be compliant with the clinical governance requirements of the Community Pharmacy Contractual Framework (CPCF).
- Staff who will provide the service must be competent to provide the service (see service specific sections on training requirements and resources for further details).
- Where the pharmacy owner is registered to provide COVID-19 vaccinations and a patient is aged under 18 years, or if COVID-19 or adult influenza vaccinations are to be undertaken in the patient’s own home, those involved in this vaccination activity must have an enhanced Disclosure and Barring Service (DBS) check against the adult and children’s barred list.
Other requirements or matters that pharmacy owners should consider before providing each of the services can be found below:
COVID-19 vaccination
COVID-19 Programme Updates and Clinical Guidance (Futures platform)
NHS England Seasonal Vaccination Provider Programme Guide (Futures platform)
Adult flu vaccination
Download the pharmacy owner checklist for the NHS Adult Flu Vaccination Service
This checklist provides suggested actions that pharmacy owners need to undertake to prepare to provide the service.
Pharmacy professional checklist
Download the vaccinator implementation checklist for the NHS Adult Flu Vaccination Service
This checklist provides suggested actions that vaccinators need to undertake to prepare to provide the service.
Standard Operating Procedure (SOP)
Pharmacy owners must have an SOP in place for provision of the service, having regard to the requirements of the legal framework(s) used to administer vaccines, the service specification, and which covers the following points as a minimum:
- The provision of the service to patients and the roles of different staff members, including the training required for staff members;
- The ongoing conditions under which the service needs to be provided (set out in the service specification);
- Cold chain integrity;
- Needle stick injuries;
- The process for escalating any issues identified during provision of the service and signposting details that can be used to guide parents/guardians to further support, where needed;
- The identification and management of adverse reactions;
- Record keeping requirements;
- The handling, removal and safe disposal of any clinical waste related to the provision of the service.
Premises requirements
The pharmacy must have a consultation room in which to provide the service, which meets the requirements of the Terms of Service.
The exception to this requirement is for distance selling premises (DSP) pharmacies, as they cannot provide this service face-to-face with patients at the pharmacy premises, so do not need a consultation room at the pharmacy.
Vaccinations must take place in the consultation room wherever the patient expresses this preference.
Vaccinations can also be offered in any area of the pharmacy where suitable facilities are available, infection prevention and control standards can be maintained and patient confidentiality and dignity is able to be respected.
Pharmacy owners must appropriately dispose of any clinical waste or personal protective equipment (PPE) used during the vaccination process and will therefore need to ensure they have contracted for a suitable waste disposal service for their pharmacy premises.
Professional oversight
The responsible pharmacist at the registered pharmacy premises is professionally responsible for overseeing this service.
If the responsible pharmacist is unable to provide sufficient oversight, for example due to workload or where vaccinations are undertaken off the pharmacy premises, an on-site pharmacist or pharmacy technician responsible for the delivery of the service must be linked and work closely with the Responsible Pharmacist and Superintendent Pharmacist through an appropriate governance framework to ensure appropriate oversight of the service.
National Booking Service (NBS)
NBS will be used by patients to book COVID-19 vaccination appointments and may be used to book flu vaccinations at pharmacies where enabled by pharmacy owners.
Pharmacy owners must offer COVID-19 vaccinations through NBS to patients and must comply with minimum publication standards for NBS appointments set out in the service specification. These include ensuring that:
- Accurate information is published and appointment or clinic times are uploaded in a timely way to allow patient bookings to be taken;
- At least 100 appointments are listed in the first month after the COVID-19 vaccination service commencement date; and
- At least 50 appointments are subsequently listed per month.
NHS England can choose to pause, reduce or withdraw COVID-19 vaccine supply to any pharmacy owner that fails to maintain compliance with the requirements of NBS set out in the service specification.
Vaccination appointments and clinics should provide maximum flexibility for patients and should be available at a range of times throughout the pharmacy’s full opening hours including, where appropriate, late afternoons and Saturdays (where the pharmacy contractor is open on Saturdays) to maximise vaccination uptake to eligible cohorts.
Manage your Appointments on NBS
Manage Your Appointments (MYA) is the new appointment management system for sites to manage vaccination availability on the NBS. It replaced Q-Flow in August 2025. The NBS currently supports COVID-19, flu and RSV. Pharmacy owners must obtain the correct contracts and assurances with commissioners before publishing vaccination availability.
Access guidance on MYA (FutureNHS login required)
Federated Data Platform (FDP)
Pharmacy owners taking part in the spring COVID-19 vaccination programme will require Federated Data Platform (FDP) access to order COVID-19 vaccines. Pharmacy owners can request FDP access here.
A step-by-step guide is also available.
If access issues occur, pharmacy owners should clear their browser cache, switch to Microsoft Edge or use an InPrivate/Incognito window and paste the link directly into the address bar. Persistent issues are typically caused by local firewall settings; pharmacies who are part of a pharmacy chain may need to contact their local IT Service Desk for assistance.
FDP access drop-in sessions
FDP Access drop-in sessions (Future NHS log-in required) are available on:
- 23rd February 2026 from 11:00am to 11:30am;
- 27th February 2026 from 2:00pm to 2:30pm; and
- 10th March 2026 from 12:00pm to 12:30pm.
Each session covers the same content, therefore, pharmacy owners will only need to attend one session. Before attending, pharmacy owners are advised to log into FDP ahead of their training session so they can follow along with the demonstrations.
Walk-in clinics
Pharmacy owners must offer vaccinations through advertised walk-in clinics via the NHS Pharmacy Services Finder for both COVID-19 vaccinations and adult flu vaccinations during the commissioned service period.
Pharmacy owners should consider when these walk-in clinic times are offered to ensure they promote access to the service.
Provision of the services off the pharmacy premises
Vaccinations can also be undertaken in other suitable locations, such as in the patient’s home or community venues (e.g. community centres).
Pharmacy owners, including DSP pharmacy owners, who want to provide an off-site service must obtain consent from the NHS England regional vaccinations team if they wish to carry out vaccinations at a location off the pharmacy premises.
There are various matters that a pharmacy owner will need to consider ahead of any provision of the service off the pharmacy premises, including:
Professional oversight: Where vaccinations are undertaken off the pharmacy premises, pharmacy owners must ensure there is an on-site pharmacist or pharmacy technician responsible for the provision of the service (or providing the vaccination service themselves) and who will ensure provision of the service is in line with the requirements of the service specification.
The setting used for vaccination: pharmacy owners must ensure that the setting used to administer the vaccinations is appropriate, including ensuring patient confidentiality and dignity.
Support staff: vaccinators should consider being accompanied by a trained pharmacy support staff member. The primary role of the support staff member would be to assist in the event of an emergency, but they could also undertake administrative tasks and, where necessary, act as a chaperone.
Clinical waste: pharmacy owners must appropriately dispose of any clinical waste or personal protective equipment (PPE) used during the vaccination process. That should include ensuring they meet the requirements of waste disposal legislation in relation to transferring waste from the site of vaccination back to the pharmacy premises for subsequent safe disposal.
Maintaining the cold chain: vaccinators must ensure that the cold chain storage of the vaccines is maintained. Vaccines should be taken from the pharmacy fridge and placed into an appropriate validated cool box (which will maintain the vaccines at a temperature between 2˚C and 8˚C) just before travel to the off-site location.
The vaccines should be kept in their packaging and should be insulated from the cooling system within the cool box, e.g. using bubble wrap, to avoid the risk of freezing.
Professional standards: when considering any provision of vaccination services outside the pharmacy, pharmacy owners and their pharmacists/pharmacy technicians must ensure they continue to comply with all professional standards.
Any planning or risk assessments undertaken ahead of off-site provision need to keep these standards central to considerations of how to provide the service, as they will offer a useful framework to help decision making.
Indemnity insurance: pharmacy owners must ensure their professional indemnity cover applies to provision of the service off the pharmacy premises.
Staff providing the service and administering vaccines will need to be authorised to operate under the appropriate legal framework. That means the service will generally be provided by pharmacists and pharmacy technicians within community pharmacies, but other registered healthcare professionals/staff able to operate under the appropriate legal mechanism (PGD / national protocol) may also administer vaccines.
Any pharmacy staff involved in the provision of the service should receive appropriate training relevant to the role they will undertake.
Vaccinators must complete the specific modules on COVID-19 vaccinations and influenza vaccinations which are available on the e-learning for healthcare website, where general immunisation training modules can also be accessed.
Pharmacy owners are required to demonstrate that all staff providing the service in their pharmacy have the skills and knowledge needed to do so. This includes working within the relevant systems and processes set out by the pharmacy owner and understanding how to report concerns, should any be identified.
The content of training for vaccinators
Vaccinators providing the service must have undertaken appropriate training in line with the National minimum standards and core curriculum for vaccination training.
This document describes the training that should be given to all practitioners engaging in any aspect of immunisation so that they are able to confidently, competently and effectively promote and administer vaccinations.
The document was updated in June 2025 and replaces the previous training standards for registered healthcare practitioners and healthcare support workers.
Pharmacists, pharmacy technicians and other vaccinators who will administer flu vaccines must have completed practical training in vaccination that meets the requirements set out in the document.
The frequency of training
Pharmacists, pharmacy technicians and other vaccinators providing the service need to attend face-to-face refresher training periodically.
This refresher training should help to ensure consistency of practice, provide peer support and allow discussion of any clinical issues that are arising in practice.
Pharmacy owners and vaccinators need to consider when it would be appropriate to attend refresher training or if ongoing competence of an individual vaccinator can be evidenced, without the need for face-to-face training.
An individual’s continued competence may be influenced by their prior experience vaccinating patients, including the overall number of vaccines administered and the regularity with which they administer vaccines.
Understanding the relevant clinical guidance
The service specification requires that the pharmacy owner ensures vaccinators have read and understood the clinical guidance available in relation to the service and that they have processes in place to check any updates to these documents.
The key sources of clinical guidance in relation to these services will be:
COVID-19: the green book chapter 14a
Influenza: the green book chapter 19
The legal frameworks to support the services (PGDs and national protocols) are developed by UKHSA and will be published before the commencement of each vaccination campaign period.
Annual update training
Vaccinators are expected to undertake annual update training, to ensure their knowledge stays up to date with changes in practice and guidance.
This may involve self-directed learning, using relevant references sources, such as the Green Book and the annual flu letter. It may also include online training which is available from a range of providers.
Assessment of vaccinator competency
The National minimum standards and core curriculum for vaccination training recommends that immunisers should keep a portfolio of completed competency checklists, knowledge test score sheets, reflective logs, completion of e-learning course certificates and certificates of attendance at immunisation training courses and updates.
This will provide vaccinators with a means to be able to show evidence of completion of training and achievement of competence to both current and future employers. It will also provide useful evidence of continuing professional development for professional revalidation.
Pharmacy owners must ensure that vaccinators are competent to provide the service and they must keep evidence of competency relating to any staff that they employ or engage to provide the service.
The Declaration of Competence (DoC) approach, using the Vaccination Services DoC (hosted on the Centre for Pharmacy Postgraduate Education (CPPE) website) is one way which pharmacy professionals providing the service can demonstrate their competence to the pharmacy owner.
Alternatively, the competence of any vaccinators can be assured using the National minimum standards and core curriculum for vaccination training competency assessment tool in appendix A of the guidance.
This can be used as a self-assessment tool, an assessment tool for use with a supervisor or both, depending on the previous experience of the vaccinator.
The recommendations that accompany the assessment tool advise that all new vaccinators should complete the competency assessment for formal assessment and sign-off of their clinical competency.
Any vaccinators returning to vaccination after a prolonged interval should also complete appropriate update training and the appropriate vaccination competency assessment. As the circumstances and training needs for individual practitioners returning to vaccination will vary, there is no defined time interval for ‘prolonged’, but vaccinators and their supervisors need to be assured of their competence before they provide the service.
General training resources
CPPE Immunisation resources
This is a CPPE gateway page that provides access to a variety of e-learning programmes and resources. The page includes links to some of their e-learning programmes that support vaccination. Their programmes are developed for pharmacists, pharmacy technicians and foundation trainee pharmacists.
Vaccinators must complete the specific modules on COVID-19 vaccinations and influenza vaccinations which are available on the e-learning for healthcare website, where general immunisation training modules can also be accessed.
Training providers
There are several organisations that provide vaccination training and those that we have been made aware of are listed below for information.
Listing on this page does not constitute endorsement of the course or provider by Community Pharmacy England.
AAH Pharmaceuticals (Account required)
Alliance Healthcare – Skills in Healthcare (Account required)
Avicenna (Login required)
National Pharmacy Association (Members login required)
Numark (Members login required)
Pharmacy team training
The whole pharmacy team can proactively promote uptake of vaccinations provided by this service. Teams should be briefed on the service and coached on how to best approach people about the service. Speak to your LPC to confirm if they have any locally arranged training to support pharmacy staff.
This section contains additional information and resources to support pharmacy owners and their teams to provide the Seasonal Vaccination Services.
Community Pharmacy England resources
To review the range of additional resources which pharmacy owners can use to assist with their understanding, implementation and provision of these vaccinations to patients, please refer to each the individual vaccination sections.
COVID-19 vaccination
Resources will be developed in due course.
Adult flu vaccination
Implementation guidance:
Pharmacy owner checklist for the NHS Adult Flu Vaccination Service
A checklist to help pharmacy owners to prepare for and to provide the service.
Vaccinator implementation checklist for the NHS Adult Flu Vaccination Service
This checklist provides suggested actions that vaccinators need to undertake to prepare to provide the service.
Joint guidance and briefing documents
National flu immunisation programme letter 2026/27 (the Annual Flu letter) (updated 26th February 2026)
Update to the Annual flu letter (published on 28th July 2025)
NHS England resources
Letter: 2026/27 COVID-19 and adult influenza vaccination service specification now published for community pharmacy
This letter summarises the key changes to the COVID-19 and adult flu service specifications for 2026/27. It includes details of the item of service fees for COVID-19 and adult flu vaccinations, the service registration process and deadlines and any changes in service requirements pharmacy owners should be aware of.
Seasonal Vaccination Provider Programme Guide- Spring 2026 (Futures platform)
Seasonal Vaccinations Site Campaign Guide AW2026/2027 (Future NHS log-in required) (Awaiting publication)
COVID-19 vaccination programme hub (FutureNHS collaboration platform)
If you do not have access to the Future NHS platform, you can register directly on the site using an NHSmail @nhs.net or similar recognised email address.
UKHSA guidance and briefing documents
COVID-19 vaccination
COVID-19: the green book chapter 14a
COVID-19 vaccination: information for healthcare practitioners
Guidance for healthcare practitioners about the COVID-19 vaccination programme. (Updated 10th September 2025)
COVID-19 vaccination: vaccine product information (Updated 10th April 2024)
Information on the presentation, doses and storage of COVID-19 vaccines.
Adult flu vaccination
Influenza: the green book chapter 19
UKHSA annual flu programme website hub
Influenza vaccines marketed in the UK Influenza vaccines marketed in the UK for 2026/27, including ovalbumin content (26th February 2026)
Flu vaccination programme: information for healthcare practitioners
Flu immunisation for social care staff
General guidance
UKHSA Immunisation website hub
Protocol for ordering, storing and handling vaccines
Vaccination of individuals with uncertain or incomplete immunisation
Vaccine incident guidance: responding to errors in vaccine storage, handling and administration
DHSC guidance and briefing documents
JCVI statement on influenza vaccines for 2026 to 2027 (12th November 2025)
This document sets out JCVI’s scientific view on the use of influenza vaccines in the UK for the 2026 to 2027 influenza season.
Other resources
Anaphylaxis action card – Personalise this card and keep it by the phone to guide staff on calling an ambulance if a patient has an anaphylactic reaction to a vaccine.
Anaphylactic guidelines and algorithm poster (Resuscitation Council UK) (May 2021)
NICE – Guideline 103, Flu vaccination: increasing uptake (August 2018)
This section provides information on some of the practical requirements related to provision of the service.
Patient consent
As with the provision of any pharmacy service, prior to vaccination, informed verbal consent must be sought from the patient or the parent/guardian of each patient for the administration of the vaccine.
Informed consent should be recorded in the pharmacy’s clinical record, including the name of persons that have consented on the patient’s behalf and that person’s relationship to the patient.
The General Pharmaceutical Council’s Guidance on Consent provides further information on consent for pharmacists and their teams.
The patient or the parent/guardian of each patient should also be advised of the information sharing that will take place for the appropriate recording of the vaccination in the patient’s GP practice record and information that will be shared with NHS England and the NHSBSA as part of post-payment verification (PPV).
Service records, IT support and sharing of data
Pharmacy owners must use an NHS-assured Point of Care System to record the administration of vaccinations.
For the 2026/27 vaccination season, NHS England has agreed to fund the cost of the Point of Care System, with pharmacy owners able to select a system of their choice from the list of NHS-assured systems.
IT suppliers listed on the Point of Care (PoC) IT Supplier Contractual Framework will be assured by NHS England as having met specific minimum standards. Community pharmacy owners carrying out these services will be able to choose, one of the assured PoC systems.
Pharmacy owners are able to choose from the following five PoC systems:
- Cegedim’s Pharmacy Services;
- Optum (formerly EMIS) Pinnacle Outcomes4Health;
- Positive Solutions HxConsult;
- RAVS (the NHS ‘in-house’ Record A Vaccination Service platform); or
- Sonar
Choosing your PoC supplier and supplier information and webinars
Pharmacy owners can find information (including some webinar recordings) that explain the different systems and offerings: Futures platform: Pharmacy PoC hub (FutureNHS login required)
General requirements related to record keeping:
- Pharmacy owners must maintain appropriate electronic records to ensure effective ongoing service delivery. Records must be managed in line with the Records Management Code of Practice for Health and Social Care.
- Pharmacy owners must ensure that the vaccination event is recorded on the same day that it is administered unless exceptional circumstances apply.
- Pharmacy owners must ensure vaccination records are complete and include all of the required fields about the patient.
- Pharmacy owners must ensure that any staff recording the administration of the vaccination have received relevant training to be able to update records appropriately and accurately.
- Where the Point of Care System is unavailable due to exceptional circumstances beyond the control of the pharmacy owner, then the record of vaccination events must be added to it as soon as possible after the system becomes available again.
- Where a record of a vaccination needs amending or has not been created on the point of care system, the pharmacy owner is responsible for undertaking the amendment or creation as soon as reasonably possible following notification from the patient or another healthcare professional that the record is not complete or correct.
Use of Point of Care IT systems:
- There must be robust user and access management processes to ensure high levels of security in relation to staff access to the Point of Care System. That should include frequent updates to system access levels to add users who join the pharmacy team or remove accounts where staff leave or do not have shifts scheduled at the pharmacy.
- Only one Point of Care System can be used to record vaccinations in any calendar month except where it is necessary to make amendments to previously recorded vaccination events or where this has been agreed with NHS England during the transition to a new Point of Care System.
Retention of records:
- Records must be managed in line with the Records Management Code of Practice for Health and Social Care.
- The necessary records required for reimbursement must be kept for a period of three years to demonstrate the service was delivered in accordance with the service specification, and to assist with PPV activities. These records must be provided by a pharmacy owner when requested by the NHSBSA Provider Assurance Team.
- Pharmacy owners should ensure that clinical records for the service are retained for the appropriate period. This retention period may be beyond the specified period for PPV purposes and should be in line with both the requirements for the record type and the age of the person being vaccinated. You can find links to further guidance on this topic on our Data handling, record keeping and disposal webpage.
Sharing of data:
- Data recorded via the Point of Care System regarding the patient’s vaccination will be shared with the patient’s registered general practice (where this is known) automatically on the day of provision or on the following working day. This will be sent as a structured message in real-time by the point of care system.
- If the structured message system is not available or fails, the pharmacy owner must ensure a copy of the vaccination notification is sent or emailed (via NHSmail) to the patient’s registered general practice as soon as reasonably possible.
- Some of the data recorded in the Point of Care System will be shared via an application programming interface (API) with the NHSBSA’s MYS platform as part of normal payment arrangements.
- Pharmacy owners must promptly comply with any reasonable request for information from NHS England (or an organisation acting on their behalf) relating to this service.
- Personal data recorded in Point of Care Systems will flow to NHS England for managing and monitoring vaccination programmes; it will also be shared with the UKHSA under a Data Sharing Agreement.
- Data that has been pseudonymised may be used by the NHS for evaluation and research purposes.
Storage of vaccines
Vaccines should be stored in line with the requirements set out by their manufacturer in the Summary of Product Characteristics.
In 2014, Public Health England issued guidance on the protocol for ordering, storing and handling vaccines for all healthcare providers involved in vaccinations, including community pharmacies.
All refrigerators in which vaccines are stored must have a maximum / minimum thermometer. Readings must be taken and recorded from the thermometer on all working days and appropriate action taken in a timely manner when readings are outside the recommended temperature range.
Safeguarding
During the consultation, if there are concerns about a potential safeguarding issue, then appropriate action should be taken, where necessary, in line with local safeguarding processes.
Guidance on safeguarding can be found in NHS England’s Safeguarding App/website.
Your Local Pharmaceutical Committee may also have details of local safeguarding contacts on their website.
Clinical waste
Pharmacy owners are required to make arrangements for the removal and safe disposal of any clinical waste and PPE related to the provision of this service. This includes where vaccinations are carried out off-site or in a patient’s home.
Where a pharmacy owner chooses to provide COVID-19 vaccinations as part of this service, the local Integrated Care Board should commission clinical waste collections for the COVID-19 vaccination service (as was previously the case for the standalone COVID-19 vaccination service).
Pharmacy owners must also ensure that staff are appropriately trained and made aware of the risks associated with the handling and disposal of clinical waste and that correct procedures are used to minimise those risks.
A needle stick injury procedure must be in place.
Communicating and working with GP practices
When pharmacy teams provide the service, notifying the patient’s GP practice of the administration of the vaccine is an important service requirement.
Data recorded via the Point of Care IT System regarding the patient’s vaccination will be shared with the patient’s registered general practice automatically on the day of provision or on the following working day. This will be sent as a structured message in real-time by the point of care system.
If the structured message system is not available or fails, the pharmacy owner must ensure a copy of the vaccination notification is sent or emailed (via NHSmail) to the patient’s registered general practice as soon as reasonably possible.
Where a patient presents with an adverse drug reaction following the initial vaccination and the pharmacist believes this is of clinical significance, such that the patient’s general practice should be informed, this information should be shared with the general practice as soon as possible.
Dealing with local issues related to the service
Sometimes issues with the service may arise between general practices and community pharmacies; in this situation pharmacy owners may wish to seek support and advice from their LPC.
Occasionally, we receive reports of general practices issuing information to their patients that unfairly or inaccurately represents the community pharmacy service. If this occurs, we advise pharmacy owners to raise the issue with the general practice concerned. If that does not resolve the issue, pharmacy owners should raise the matter with the Integrated Care Board primary care contracting team and their LPC.
Sometimes examples of such information get circulated via social media and other routes, which can create a larger issue from a single incident than may be warranted and it also potentially inspires others to copy the approach. We recommend that LPCs and pharmacy teams avoid sharing such matters via social media, as it will not help long term community pharmacy/general practice relationships; incidents should be dealt with locally wherever possible.
Dealing with incidents arising from the provision of the service
If an incident occurs in relation to the service, pharmacy owners are required to report any patient safety incidents in line with the Clinical Governance Approved Particulars for pharmacies.
Where necessary, the pharmacy owner is also expected to follow UKHSA’s Vaccine incident guidance: responding to errors in vaccine storage, handling and administration.
Withdrawal from provision of the service
If a pharmacy owner wishes to stop providing the service, they must notify NHS England that they are no longer going to provide the service giving 30 days’ notice prior to cessation of the service via an electronic declaration form to de-register before 31st March 2026. This is an interim arrangement until MYS registration is available in April 2026.
From 1st April 2026 onwards, pharmacy owners who wish to de-register from the service can do so via their MYS portal.
They must continue to provide the service for the duration of the notice period. Pharmacy owners that de-register before the service commencement date are not required to give 30 days’ notice.
Pharmacy owners must ensure they update NBS and NHS Profile Manager when they cease provision of the service.
If a pharmacy owner de-registers from the service, they will be unable to re-register for a period of 4 months from the date of de-registration.
To review resources that are available to promote the vaccinations, please refer to each the individual vaccination section below.
COVID-19 vaccination
Shared Learning & Equalities
A range of bespoke tools, resources and content for your engagement and practice in supporting and learning from people and partners within underserved communities and equalities groups has been published on the Futures platform.
Posters and resources
Signposting patients
A service finder, on the NHS website, lets members of the public and healthcare professionals search for a pharmacy that offers a walk-in vaccination service.
Find a walk-in COVID-19 vaccination site – NHS
Members of the public can also book, amend or cancel appointments online or via their NHS App.
Book, change, or cancel a COVID-19 vaccination appointment online
Adult flu vaccination
We have developed a range of materials which pharmacy owners can use to promote the availability of this service to patients.
Our shared folder (link below) allows you to download the latest versions of the following resources:
- Posters for display (both ready to use and editable versions);
- Suggested social media graphics and messages;
- Letters to eligible patients and local care providers;
- Flyers for attaching to prescription bags;
- Template local press releases;
- Radio scripts; and
- Materials to support hosting an MP pharmacy flu jab visit.
Download here: Flu Vaccination Service promotional materials
UKHSA resources
Leaflets
The below listed leaflets are also available in Albanian, Arabic, Bengali, Bulgarian, Chinese (simplified), Cantonese (traditional, Cantonese), Estonian, Farsi, French, Greek, Gujarati, Hindi, Latvian, Lithuanian, Panjabi, Pashto, Polish, Portuguese, Romanian, Romany, Russian, Somali, Spanish, Tagalog, Tigrinya, Turkish, Twi, Ukrainian, Urdu, Yiddish and Yoruba via the below links.
UKHSA patient leaflet – Flu vaccination: who should have it this winter and why
UKHSA flu leaflet for pregnant women
Copies of these leaflets can be ordered from the Health Publications Order point or by phoning 0300 123 1002 and quoting the reference numbers on the back pages of the leaflets.
Flu immunisation for social care staff
Leaflets for social care staff and providers to support the annual flu programme.
Posters
A quick links poster with QR codes to the Pregnancy: how to help protect you and your baby (the leaflet describes the vaccines, including the flu vaccine, that are recommended during pregnancy) and the COVID-19 vaccination: a guide on pregnancy and breastfeeding leaflets (2021)
National invitations to present for vaccination sent by NHS England to patients will include information about the pharmacy offer and details of how to book an appointment at a pharmacy via NBS.
Developing your own marketing materials
If pharmacy owners decide to develop their own marketing materials to promote the service they must ensure they comply with the requirements of the Terms of Service relating to promotion of services funded by the NHS.
If pharmacy owners choose to use the NHS identity on their marketing materials they must follow the primary care guidelines for use of the NHS identity.
An A-Z style guide of words and phrases about health and the NHS, which aims to make content aimed at patients easy to understand, is available on the NHS website. The NHS website team try to use words on their website that people use themselves when they talk about their problems and when they search for information on the internet. Community pharmacy teams may wish to refer to the guide when producing their own health content or communication materials.
Identifying carers eligible for a flu vaccination
Small carer flu vaccination flyers
These double-sided flyers can be attached to prescription bags and be used as a conversation starter to encourage carers to have a flu vaccination.
We have previously worked with Carers Trust and they produced ‘ten signs that tell community pharmacy teams that someone may be a carer’. These are listed in the box below:
Carers are often the people who:
|
Flu vaccinations for people with learning disabilities
People with learning disabilities are eligible to receive a flu vaccination under the service, as learning disabilities are categorised as a neurological condition.
Around 1 in 3 deaths of people with a learning disability are caused by respiratory problems and the number of respiratory related deaths increases during winter. Having the vaccination can help avoid preventable deaths for people with a learning disability during this period.
A person with learning disabilities will have:
- a significantly reduced ability to understand new or complex information and to learn new skills (impaired intelligence); and
- a reduced ability to cope independently (impaired social functioning).
This will have started before adulthood, with a lasting effect on development. This does not include conditions like dyslexia, which cause a specific difficulty with one type of skill but not a wider intellectual impairment.
People with learning disabilities are less likely to get flu if the people around them are also vaccinated; carers and care workers are eligible to receive a flu vaccination under the service.
UKHSA has easy read flu resources, which are aimed at people who have, or care for someone with a learning disability.
Suggested actions to improve flu vaccination uptake amongst people with learning disabilities:
- Ensure you continue to talk to people in general about getting a flu jab so people with learning disabilities are aware that they can get a flu vaccination from the pharmacy;
- Let carers of people with a learning disability know that they are also entitled to an NHS flu vaccination to protect the person they are caring for;
- Ensure the eligibility criteria you have displayed (on your website or in the pharmacy) for the service or any patient materials, include learning disabilities as an eligible group;
- Consider the information you display in your pharmacy to promote the service to this eligible group of patients – can it be easily read and understood by all your patients?
- Consider undertaking some learning to enhance your understanding around people with learning disabilities; the Centre for Pharmacy Postgraduate Education has a distance learning course available.
- If a person has a learning disability, annotate their PMR to indicate their eligibility for an NHS flu vaccine so you can talk to them about being vaccinated when the service commences again in the autumn.
- Understand your responsibilities under the Mental Capacity Act to ensure appropriate consent is captured or where necessary, an appropriate capacity assessment can be carried out.
Other resources
People with learning disabilities and the flu injection
Easy-read information with information for people with learning disabilities, their family, carers and paid supporters (National Development Team for Inclusion).
NHS England short video on flu vaccination for people with a learning disability and autistic people
The video covers why it is important eligible people have a flu vaccination, who is eligible for a free vaccine, reasonable adjustments, consent and decision making. A parent of a 16-year-old with a learning disability describes how primary care can support families to make sure their relatives can have their vaccination.
The flu jab for people with learning disabilities
YouTube video showing a patient with learning disabilities having a flu vaccination (NHS England).
Pharmacy and people with learning disabilities: making reasonable adjustments to services
Guidance on how to make reasonable adjustments to help support people with learning disabilities in using pharmacy services.
Pharmacy owners will be paid:
- £10.06 for each adult flu vaccine provided in 2026/27;
- £8.70 per COVID-19 vaccine administered between 1st September 2026 and 31st January 2027 while the flu vaccination campaign is underway; and
- £10.06 outside the flu vaccination campaign period.
These fees are funded from NHS vaccination budgets, not from the CPCF global sum.
COVID-19 vaccinations are supplied free of charge and will not be reimbursed as part of this NHS programme.
Where pharmacy owners administer the recommended flu vaccine to eligible patients under the service, they will be reimbursed for the vaccine cost at the basic price (list price) of the individual vaccine administered and an allowance at the applicable VAT rate will also be paid.
Basic prices can be confirmed using the NHS Business Services Authority’s DM+D browser.
Claiming payment
The Point of Care IT System which pharmacy owners and their teams use to make a clinical record for the service will also populate a claim for payment, via an API within the NHSBSA’s MYS portal.
The transfer of data via the API happens throughout the month, as data is entered into the IT system. The service provisions will then be available to view in MYS from the 1st of the following month.
For example, service provisions in October will be available to view in MYS on 1st November. Pharmacy owners must log into the MYS platform to check that the data matches the details in their IT system, and then must submit their claim for payment.
Pharmacy owners must claim payment within one month of, and no later than three months from the claim period for the chargeable activity provided.
Claims which relate to work completed more than three months after the claim period in question will not be paid and the pharmacy owner will not receive any payment for the administration of those vaccinations.
The exception to this is where the submission of a claim was delayed by IT issues outside the pharmacy owner’s control (such as issues with the NHS approved API system used by the pharmacy owner or with the MYS portal). Such claims will be accepted outside the usual grace period within 12 months of the date by which the claim should have been submitted. This is subject to the NHSBSA receiving evidence of the IT issue, and only if investigation finds that the evidence demonstrates that the IT issue was outside the control of the pharmacy owner, and it delayed the claim submission.
Payments to pharmacy owners will be made monthly as part of their normal payment schedule.
Payment will only be made for vaccinations administered from the service commencement date to the end of the service end date.
Advance payments
Following the announcement that clinical services are now included in advance payments, the advance service payments include the consultation fees for the Adult Flu Vaccination Service. Reimbursement for the vaccines administered as part of the Adult Flu service is also factored into the calculation of the main drug advance payment itself.
The value of the ‘Service fee advance’ displayed on the payment schedule is calculated based on the activity declared via the MYS portal.
Pharmacy owners will receive service fee advances on the same day as the early advance payment for dispensed prescriptions, provided the declaration is submitted within the usual claiming deadlines. The service fee advance payment is then recovered at the end of the following month – similar to the recovery of advances paid for prescriptions.
More information on service fee advances can be found in the following news stories: Advance Payments Update: Payments now include Flu and Covid-19 activity and Service fee advances.
FAQs will be added shortly
On 21st January 2026, Community Pharmacy England and NHS England hosted a joint webinar to help pharmacy owners understand the combined service, the operational changes and stock procurement of COVID-19 vaccines.
Seasonal Vaccinations Service webinar – this webinar was aimed at helping pharmacy owners and their teams to understand the differences between the combined service and the previously commissioned services, as well as the operational requirements to provide the services.
Presenters also highlighted the requirements that pharmacy owners will need to meet prior to offering the service, as well as the guidance and resources available to support them.
At Community Pharmacy England, we are always keen to hear from pharmacy owners and their teams about how the provision of national pharmacy services is going, be that niggles with the way services are commissioned, a success story you want to share or something else.
Please click on the link below to share a success story where you have helped achieve a good outcome for a patient following a consultation for a national pharmacy service or to provide feedback on one of the services.
For more information on this topic please email services.team@cpe.org.uk